
Features
Practice
Health
Patient Care
Wellness
Breaking the loop: Causalgia
A curious case of a ‘crazy’ kind of pain, part 2
November 17, 2020 By Dawn Armstrong
 Photo: @ EdNurg / Adobe Stock
Photo: @ EdNurg / Adobe Stock Florence is a new patient we met in the Summer issue of Massage Therapy Canada. I pegged her situation as a likely case of causalgia, also known as Complex Regional Pain Syndrome (CRPS).
Because there is no single test to confirm the diagnosis, it’s a matter of taking a thorough case history and asking enough of the right questions. You also need to observe carefully as you physically examine the involved area.
Typically, there is a history of pain in a limb or a smaller part of a limb (like a thumb) or the region of distribution of a specific peripheral nerve (like the median nerve or, as in Florence’s case, the anterior femoral cutaneous nerve). And it’s not just any kind of pain. It is characteristically a burning pain and much worse than one would expect under the circumstances. The term allodynia applies, meaning that an otherwise normal stimulus produces pain that is wildly out of proportion to the situation.
The symptoms of CRPS are often constant but can present with a pattern of relative quiescence punctuated by spikes of pain that are triggered by certain things, like movement, light touch, heat or cold, vibration – even something as slight as a breeze. Some cases are relatively mild and recover spontaneously. Most cases are bad and never completely go away. Rarely, the pain worsens over time and spreads – consuming an ever-increasing area or even developing in the same part on the opposite side of the body.
In spite of all the attention that the affected area demands, patients may experience a sense of disconnection from their troublesome leg or arm – as though it is no longer “theirs.” Due to the unrelenting or unpredictable nature of their pain, a patient’s mood can swing from deep depression to intense anxiety and back, their sleep is disturbed, their will to live can falter.
Women are more likely to be affected than men. It can affect people of any age, but it is almost never seen in very young children and is uncommon in the elderly. But, the fact is that CRPS is a rather uncommon disorder across any population. Many primary healthcare providers have never seen a case.
On physical examination of the affected region you will first be looking for changes to the skin:
- Is the colour normal? Is it pale, or are there blotches of red or blue or purple?
- Is the temperature normal? You may note that the painful spot of skin or the entire limb is warmer or colder than other parts.
- Does the skin seem at all sweaty or damp?
- Do you see any textural changes such as abnormally smooth and shiny areas or mottled patches of epidermal sloughing?
When limbs or digits are involved, active range of motion of joints may be restricted; passive ROM’s can also be affected and the limitations are often in all directions.
There can be weakness on resisted testing and trouble coordinating movements. Fine tremors are not uncommon. So why did this happen to Florence? Do we suspect that her case is a result of the orthopedic surgeon making some sort of mistake? It seems significant that her problem began just two days after surgery. Certainly replacing a knee joint is a traumatic procedure but this crazy kind of pain can appear on the scene as a result of something as simple as a poke with a needle for a blood draw, so it’s not reasonable to suggest that her surgeon should or could have done anything differently.
What could be causing such intense pain and the sudomotor, vasomotor and trophic changes to the skin over Florence’s now four-year-old knee? We know that the turgor, colour and temperature of our tissues are determined by the activity of the autonomic nervous system. There is a general understanding in medical texts that all of the features of CRPS are ultimately due to abnormal microcirculation of fluids and nutrients, and that this is due to “nerve damage,” without elaborating on what’s meant by the word “damage.”
The idea that this complex pain disorder is because of damage to nerves deserves a closer look. The word indicates a breakage of structure, a disruption of the integrity of the physical substance. And if “the thing” we are talking about is a living cell, or a collection of cells (ie. tissues), we know that when these structures break and their integrity is compromised, they will be replaced (ideally) by new cells that work in the same way.
CRPS is not about damage to the structure. It is a case of damage to the function – the way the cells/tissues, structured as they are, are working. What do we mean by “work?” You make something or you move something, and if things are to be made and moved, you have to have a way to control just what work is done and when.
Enter the humble reflex arc, AKA the feedback loop. It is the fundamental design of control systems and the basis of all biological function – sensors and effectors which are linked together. There are different types of sensory nerves in the skin. Mechanoreceptors detect stretch, pressure and hair movement – all of the elements of the sense of touch. Nociceptors and thermoreceptors respond to local changes in chemistry and temperature.
The pain receptors are of two main types – fast and slow. For the fast ones (A-delta), a single action potential (AP) produces a conscious sense of sharp, prickly pain. One AP from a slow (C-type) sensory nerve is not perceived, while a volley of AP’s down these unmyelinated fibres results in a sense of intolerable pain. The former tell us about the time and location of the injury, the latter define its extent.
The motor nerves to the skin are predominately (if not exclusively) sympathetic motor fibres.(1) These efferent autonomic nerves release signaling chemicals – neurotransmitters/vasoactive amines – which instigate action in target tissues such as muscle and glands (sweat/sebaceous).
The muscle cells of the skin are of the smooth variety. They are found at the base of hair follicles and within the walls of arterioles, which feed the capillary beds of the dermis. When action is initiated by increased sympathetic motor activity, observable things happen.
- Smooth muscle cells contract to make hair stand on end or blood vessels constrict
- Adventitial cells which envelope the capillaries act to alter the permeability of the vascular beds
- Glands are stimulated to increase synthetic and secretory functions
So there you have it – all of the elements of a feedback loop. Afferent signals from nociceptors (fast and slow) and mechanoreceptors are linked via the central nervous system (in simple or not-so-simple ways) to sympathetic efferents, which signal the effector tissues (smooth muscle cells, glands, adventitia) to act. Depending on the location of the sensors and the type of effector involved in the motor response, we can describe reflex loops as somato-somatic, viscero-visceral, somato-visceral and viscero-somatic. A vast majority of reflex/feedback loops are of the negative type. Much like your home heating system with a thermostat, the end product – be it a substance or a movement or heat– turns the process off. Mission accomplished.
There are only a few examples of positive feedback loops. When the end product incites more action and the system spirals into a self-perpetuating cycle, things can become extreme. Like the way they do when a woman gives birth and the uterine smooth muscles contract with ever-increasing frequency and intensity against the rising pressure within the uterus – which is happening because of the contractions. Or, the way hyperthermia becomes heat stroke – the warmer the room, the more the vasculature to the skin opens up to dissipate excessive body heat, but the blood picks up more heat, the skin flushes even more and body temperature will rise to fatal levels without treatment.
What about the way a wrong move turns into muscle spasms? The sensitivity of stretch receptors turns up and the alpha-gamma co-activation loop locks into a cycle of muscle contraction, perpetuated by sensory endings within the muscle spindles which are reporting on the stretch of the sensory endings that is being created by the hypertonicity of the muscle itself. We’ve all seen this one!
In each case, the result of the body’s actions – increased smooth muscle contractility, cutaneous vasodilation, skeletal muscle hypertonicity – causes more of it to happen.
The system becomes “stuck on high.” And this, I propose, is the nature of CRPS – a somato-visceral reflex loop that is stuck and self-perpetuating. With reflex loops, like the chicken and the egg, it can be difficult to know which came first – the painful stimulus or the hyperactivity of the sympathetic motor system – but the results are obvious.
Whatever the primary lesion (and there are times when none can be identified) – be it a broken ankle or shoulder bursitis or surgery – we often see immobilization of the area, spontaneously because it hurts or deliberately because it is necessary.
Perhaps it requires a physiologic pre-disposition, plus some stressful circumstances and a perfect storm of conditions, but there is an uptick in sympathetic nervous system activity.
When sympathetic activity is turned up too high, the effects are felt throughout the involved tissues. Increasing sympathetic motor impulses causes vasoconstriction of arterioles, which produces ischemia and, simultaneously, makes the capillary beds more permeable. This leakiness affects the interstitial fluid compartment and impairs movements of nutrients and wastes. This explains the coolness and colour changes and altered texture that we can see. The dampness of the skin is because of increased motor messages to sweat glands.
The effect on peripheral sensory receptors is to exaggerate their sensitivity. The threshold of firing is lowered so they report a greater intensity of stimulus than is actually occurring. These effects can be local, regional or segmental. This process of sensitization not only affects the sensory receptors of the periphery, it happens centrally as well. Layers of integration and influence are provided by the brain and spinal cord, essentially creating dysfunctional reflex loops that can be highly complicated. (2)
There are generalized effects, too. The central nervous system expresses it with symptoms like hyper-reflexia, hyper-vigilance and insomnia. Cardiovascular signs of hyper-sympathetic tone are increased heart rate and blood pressure.
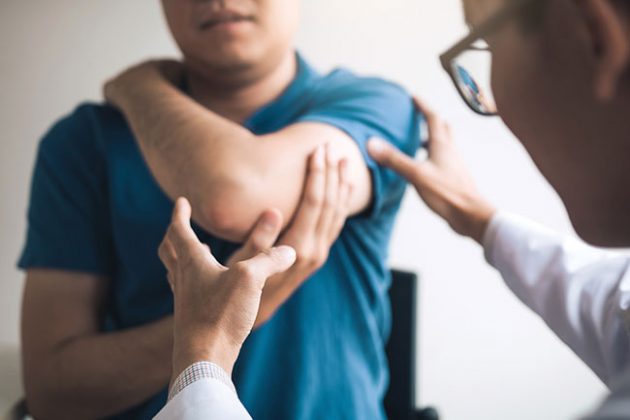
Photo: @ wutzkoh / Adobe Stock
How do all these facts reveal possible ways to help a patient like Florence? How do you stop a cycle of sensory-motor activity that is stuck in a self-perpetuating loop? You interrupt it; you break the loop. The most common medical treatment is pharmaceuticals to dampen the pain messages and relieve associated insomnia. Drugs can help a patient cope but they don’t ‘fix’ the condition. The most radical medical approach is a sympathectomy – where the affected motor nerves/ganglia are disconnected surgically or chemically.
Counselling and pain management strategies can be helpful. Coping with chronic, severe pain is challenging and exhausting; connecting with professionals who specialize in cognitive and behavioural approaches is often recommended. But, if it can be done, fixing the source of the pain has to be the most sensible thing to do. We need to correct the dysfunction.
Amongst a list of many possible contributors in painful conditions, Dr. Claraco provides some insight for us: “a lack of sufficient non-noxious information from segments related to the kinetic chain – including proximal and distal joints, synergistic and antagonistic muscles.” (3) This includes information on stretch, pressure, temperature, vibration and movement in general.
So this is what we need to do – provide these kinds of non-painful stimuli so as to change sympathetic motor output by changing the sensory input. Massage therapy has many techniques and modalities which could be effective in helping to desensitize the nervous system and re-set dysfunctional sensory-motor loops which are perpetuating the patient’s symptoms.
Soft tissue work– Don’t touch the painful area to start with. Work on the opposite side of the body and in other unaffected areas. Any methods which tend to increase parasympathetic activity, such as warm packs and guided breathing, can encourage the sympathetic system to turn down and stimulate the release of endogenous endorphins (which will decrease the sensitivity of pain nerves by raising their threshold for firing). Craniosacral therapy could be helpful in this regard as well.
Passive motion of involved or related joints – Rhythmic movements that are predictable and soothing (such as Trager techniques) effectively provide sensory input that has been missing when a patient isn’t using a body part because of the pain.
Bowen therapy – Gentle “tweaks” to modulate sensory information from muscles and tendons.
Exercise – Provide the patient with guidance and instructions on self care; assisted active movements and carefully graded resistance exercises can improve blood flow, flexibility, strength and function.
Keep in mind that as treatment is provided, you are not only working to improve the condition of the soma – you will also be preventing or reversing the secondary changes to the central nervous system associated with chronic pain.
If you ever have the opportunity to help a patient with CRPS – whether it involves a cutaneous nerve or an entire limb – remember to properly document the details of their case. The use of pain questionnaires is highly recommended if you want to objectively assess the effectiveness of the care you provide. There are many to choose from, but be sure to have them complete the questions before you do any treatment at all and then again at predetermined intervals throughout the planned course of care.
Working together with other hands-on professionals – chiropractors, TCM specialists and physiotherapists – can also be worthwhile.
Make sure to provide your patient with clear information on the nature of their condition; explain it in terms they can understand. Honest listening and compassion and reassurance can go a long way to alleviate their suffering.
What happened to Florence? She is still trying different pain medications. After four years she finally has an appointment with a pain specialist. Her back spasms cleared up when she changed her bed and I never got the chance to do any course of treatment with her. She continues to soldier on, stoic as ever and determined to care for her husband as best she can, in spite of her crazy knee pain.
Sometimes the cases that show up on our doorstep can inspire us to re-examine our understanding of the nature of pain and give us hope that what we do can help.
References:
- Cutaneous Nervous System Michel Demarchez , www.biologiedelapeau.fr
- The Pain Puzzle: A.E.Claraco Canadian Chiropractor May 2018
- Brain Pain Supply: A.E. Claraco Canadian Chiropractor April 2019
DR. DAWN ARMSTRONG is a graduate of CMCC and has been in practice for over 30 years. She is currently focused on promoting life-long learning and professional development and has created a continuing education course – Clinical Record Keeping: A Hands-On Approach. Learn more at auroraeducationservices.ca.
Print this page