
Features
Collaboration
Practice
Spinal Cord Injury, Part 1
"I was about to graduate university in France; I was athletic, having taught skiing at Mont Tremblant, sailing and windsurfing in four Club Meds; I was a fashion model in Old Montreal. I couldn’t believe that this injury was permanent – I had so much going for me.”
November 2, 2011 By By Maria DiDanieli with Sean Pothier; Angela Sarro RN(EC) MN CNN(C); Tammy Scott BSc BKin
|
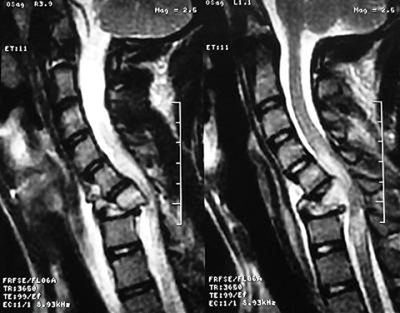
| MRI showing injury to the spinal cord.
|
" I was about to graduate university in France; I was athletic, having taught skiing at Mont Tremblant, sailing and windsurfing in four Club Meds; I was a fashion model in Old Montreal. I couldn’t believe that this injury was permanent – I had so much going for me.”

|
|
| Sean Pothier is a Voices for Injury Prevention (VIP) volunteer spokesperson for ThinkFirst Canada.
|
When Sean Pothier, a resident of Montreal and an avid volunteer spokesperson with ThinkFirst Canada – a nationwide program dedicated to the prevention of spinal cord and brain injuries – looks back, coming to terms with the permanence of his injury was the biggest wall he remembers climbing. It was through ThinkFirst that Sean encountered Rick Hansen, who is well known for a spinal cord injury (SCI) that landed him in a wheelchair at the age of 15, but well loved and respected for his accomplishments after that. Pothier tells Massage Therapy Canada that, while he was still struggling with the fact that his own injury was for life, he derived a new direction from Hansen, who said to him, “Sean, like mine, your life has changed forever. So, never look at things that you used to be able to do. Now, you have to enjoy things that you can do in your new body. But, don’t enjoy them with your old body expectations – enjoy them with your new body and what it is able to do. You can still live the same quality as before – just don’t have the same expectations.”
May was recognized across Canada as Spinal Cord Injury and Canadian Paraplegic Association (CPA) awareness month. Aligned with the mission to raise knowledge and awareness, and in honour of injury survivors, this article will provide a multidisciplinary overview of SCI, in two parts. Part 1 will describe spinal cord injury and explore care needs, and rehabilitation goals, of injury survivors. Part 2 will examine the role massage therapy can play in spinal cord injury and discuss prevention education and how massage therapists can become involved in these initiatives.
It is not the intent of the article to be a comprehensive review of this vast and complex topic, but, rather, to provide some initial information in the hope of springboarding further, much needed, involvement by members of the massage therapy profession in this area.
INTRODUCTION AND EARLY STAGES FOLLOWING SCI
Injury to the spinal cord can occur as a result of trauma or can be precipitated by certain non-traumatic activators, including infectious or inflammatory disorders and motor neuron diseases. Traumatic injury most commonly results from motor vehicle accidents and/or sport- or recreation-related injury, but can also occur as a result of work accidents, falls, violence or birth injury. Most traumatic SCIs in Canada are reported as being sustained by males between the ages of 20 and 30 years old. Non-traumatic SCI is also seen more in males, however, for both males and females, the incidence of these increases considerably beyond the age of 55. In December 2010, Canada reported a total of 1,785 new traumatic SCIs and 2,474 new non-traumatic SCIs.
In traumatic situations, the initial factor precipitating an SCI is mechanical and involves compression and/or traction of the cord. Compression may occur due to displaced bone or bone fragments, ligaments and/or disc debris. Injury to blood vessels and cell membranes, as well as cord swelling in the area of impact, initiates a cascade of events that result in disruption of autoregulation of blood flow and axonal propagation, leading, eventually, to spinal shock. Toxins that are released through broken cell membranes in the spinal grey matter, as well as electrolyte shifts in the area of injury, spark a process of secondary injury that eventually spreads to white matter, killing viable neural cells and further disrupting axon flow at, and below, the level of impact. The processes involved in non-traumatic spinal cord injury may bear some similarity to this cascade of events but are, in their details, largely specific to the disease that is responsible for the injury.
Acute assessment of an SCI includes use of functional grading scales and imaging – mostly MRI – to determine the level(s) and extent of injury, whether the injury is complete (i.e., no sensation and/or function below the level of injury) or partial (i.e., some preservation of neural function below the level of injury) and presence of comorbidities (including brain injuries, as these are a common combination). Testing of cerebral spinal fluid may be indicated in cases of non-traumatic injury. Electrophysiology may be employed to help characterize the injury if the patient is not responsive.
Treatment, at this phase, is largely aimed at neuroprotection and sheer preservation of life. Neuroprotective strategies mostly involve focusing on the effects of secondary injury. Pharmacological agents are employed to assist with inflammation, electrolyte imbalance and removal of toxic agents – mostly glutamate – being expelled in large quantities from disrupted cells in the area of injury. Surgery may be indicated, either to remove fragments threatening the spinal canal and/or to stabilize the spine. External stabilization/traction devices have also been employed.
The post-injury course experienced by an SCI patient varies, in its many elements, from patient to patient, and requires the combined efforts of a team of practitioners and therapists in medical and rehabilitative disciplines.

|
|
| Angela Sarro, RN(EC), MN, CNN(C), is a nurse practitioner in the Spine Program at the Krembil Neuroscience Centre, Toronto Western Hospital.
|
ACUTE AND LONG-TERM COURSE AND CARE
By Angela Sarro
The early stages – Some SCI individuals will require management in the intensive care unit with ventilatory support until their respiratory function improves. If ventilation is prolonged, then a tracheostomy may be required. Invasive monitoring, including intravenous therapy, arterial lines, central venous catheters and cardiac monitoring, is not uncommon. Some individuals may be placed in halo traction to try to realign the spinal column prior to any surgical intervention. Astute nursing care during the acute phase is of utmost importance to provide the necessary day-to-day care, along with emotional support to help the individual cope with his/her injury.
Some individuals may require the placement of a nasogastric or gastrostomy tube for enteral feeding. These measures are usually temporary. The assistance of a speech language pathologist will be crucial to monitor swallowing mechanisms for safety of oral feeding. Once oral intake of nutrients is deemed safe, the diet is advanced from liquids to solid foods as tolerated.
Because sensory impairment and motor function are often affected, the SCI individual is prone to skin breakdown. The use of a special pressure-reducing mattress and a regular turning schedule, often every two hours to relieve pressure areas, is an important aid in preventing skin breakdown.
Bowel and bladder management are important aspects both in the early stages and long term. Initially while in hospital, individuals will have a Foley catheter in place. Once the individual is medically stable, the catheter is removed and the bladder is monitored for any spontaneous activity. If unable to void, an intermittent catheterization protocol is set up. An effective bladder management program is important to prevent urinary infections and allow the bladder to be emptied at a convenient time.
Prevention of infection is very important in SCI. Three common infections include urinary tract infection, pneumonia and skin breakdown. The morbidity of these three in combination could result in death due to the impact on the individual’s overall ability to combat them.
Physiotherapy and occupational therapy in the acute care phase focus on early mobilization of the individual. This will become more of a focus in rehabilitation, at which point methods for learning to become as independent as possible will be important.
Considerations in the short and long term – A spinal cord injury is a devastating event for any individual. It impacts both physical and psychological aspects of one’s day-to-day activities. An individual who was completely independent in all facets of life is now dependent on someone else to do even the simplest things.
This dependency varies based on the extent of injury. An individual with an incomplete SCI may be able to regain some of the initial loss of function to varying degrees, whereas a complete spinal cord injury will require the individual to have daily support and care for most activities throughout the remainder of their lives. Most patients require day-to-day care for bathing, turning, eating and toileting. The simplest things, such as eating, or getting in and out of bed, may require the assistance of one or more people.
Psychosocial issues faced by the SCI individual, in both the short term and the long term, include anxiety, body image disturbance, grieving, ineffective coping, a feeling of powerlessness and depression. Quite often during the acute period, individuals display feelings of anger, resentment and denial. Depending on previous coping mechanisms or situations they may have been faced with, this period varies. Essential at this time is ongoing support and reassurance by the family and health-care staff, spiritual care and outside support groups to help with coping mechanisms.
Living with an SCI can be very stressful. Stress-related symptoms can delay recovery and make other problems, such as pain and spasticity, worse. Addressing this stress with a specialist, such as a rehab psychologist, can help with the development of skills and strategies for managing it.
In the short term, survival from the injury itself is the main focus. If the trauma resulted in other injuries, the transition from acute care to rehabilitation may be prolonged. Often the biggest hurdle for individuals, following a SCI, is the acceptance of the injury and the impact it will have on their lives moving forward.
Long-term care needs of an individual with an SCI are also determined by the level and the type of injury. A tetraplegic with little or no arm function will require attendant care to a much greater degree than a paraplegic who has learned how to self-transfer, dress and perform intermittent catheterizations. Attendant care programs are available to provide assistance with routine activities of daily living due to these physical limitations. The amount of care one is able to attain will determine the degree of independence they can have.
Elements that need to be taken into consideration when looking at the long-term needs of an individual with an SCI include housing, home modifications, transportation, education and employment, income maintenance, mobility aids, and supports required to maintain an active and productive life.
The injured person’s family – It is often easy to forget about the families of SCI patients during the acute phase of admission to hospital. It is important to remember that they, too, are going through a period of trauma, more psychological than physical. Emotional support for family members is crucial so that they can remain strong to support their loved ones as they recover. Support groups for families of SCI injured individuals can help them deal with their feelings and fears about the present and the future that lies ahead of them.

|
|
| Tammy Scott, BSc Kin, is a kinesiologist at Great Lakes Physiotherapy in Simcoe, Ontario, who has worked in acute and chronic care settings.
|
REHABILITATION AND FUNCTIONAL RECOVERY
By Tammy Scott
Research findings and clinical goals – With clinical and basic science research leading to new advances and prolonged survival becoming an attainable goal in spinal cord injured patients, rehabilitation of these injuries has an increasingly important role. The primary goals of rehabilitation are prevention of secondary complications, maximization of physical functioning and reintegration into the community.
Rehabilitation following SCI is most effectively undertaken with a multidisciplinary, team-based approach. Physical therapists typically focus on lower extremity function and on difficulties with mobility, as well as address upper extremity dysfunction and difficulties in activities of daily living. While each team member has primary responsibilities, any member of a properly functioning interdisciplinary team can contribute to the resolution of any problem.
Even by itself, aggressive physical rehabilitation is a complicated area in which improvements may be attributed to many causes and mediating physiological mechanisms.
First, such rehabilitation most likely stimulates some function-restoring neuronal regeneration, adaptation, and/or reconfiguration (i.e., plasticity), and also may activate dormant but intact neurons that transverse most injury sites, even injuries clinically classified as complete. Studies suggest that only a small percentage of “turned-on” neurons are needed to regain significant function.
Second, the spinal cord itself possesses intelligence and is not completely subservient to brain oversight. Specifically, the spinal cord’s “central-pattern generator” can sustain lower-limb repetitive movement, such as walking, independent of direct brain control. Extensive training coupled with braces can result in ambulation by thoroughly stimulating this neural network.
Third, many muscles above the injury site indirectly affect ambulation, especially through the use of leg braces. For example, the latissimus dorsi muscles, innervated from the cord’s cervical region, influence pelvic-area movement and, in turn, ambulation.
Fourth, aggressive physical rehabilitation is often initiated in the first year after injury, a period in which appreciable recovery potential exists. Critics have suggested that any functional recovery, no matter how dramatic, would have happened anyway in this time period.
Project Walk – Many people with SCI who have committed to Project Walk – an intensive exercise-based recovery program developed by Ted and Tammy Dardzinksi in Carlsbad, California, that attempts to re-educate the damaged nervous system through physical stimulation, (www.projectwalk.org) – have gained function much beyond what was considered possible after injury. Project Walk focuses on developing muscle potential below the injury level. The Dardzinksis believe standard rehabilitation programs not only ignore this potential, but also contribute to its extinction by “tossing in the towel,” focusing on non-paralyzed body parts needed for adaptation to wheelchair living instead of ambulation. They also believe that extensively administered anti-spasticity medications are the equivalent of pouring water on the flickering embers of regeneration that often still exist after injury. In contrast, Project Walk’s goal is to fan these embers to promote functionality below the injury level. Believing there is a post-injury therapeutic window in which the recovery potential is greatest, Project Walk ideally would like to start treating patients relatively soon after injury. Each program is individually tailored to the client. Proponents of the program believe that, without proper stimulation and load bearing, a newly injured person will soon start losing bone density, muscle mass, and CNS functioning, which makes future recovery even more difficult. Although the program has treated many after this window, sometimes with dramatic improvements, much more effort is needed.
The average client works out three hours every other day. For people returning home, individually tailored, home-based programs are designed. Although intensive, clients are encouraged not to embrace these programs exclusively at the expense of overall life balance achieved through involvement in areas such as career, school, social life, etc.
Functional improvements include increased muscle mass, CNS activity, health and well-being, sensation and function below the injury level, occupational skills, and sweating, as well as decreased drug dependence and pain. Project Walk encourages the use of synergistic healing modalities, including acupuncture, hyperbaric oxygen therapy, standing frames, FES bikes, and other electrical stimulation that helps to maintain muscle mass and circulation; and emphasizes good nutrition.
Part 2 of this article will examine the role of massage therapy in SCI and discuss injury prevention. It will appear in the Winter 2011 issue.
Print this page