
Features
Continuing Education
Education
Amputee Rehabilitation & Care
An amputation is a physical and psychological trauma that has a profound influence on the daily life of the individual. Providing comprehensive rehabilitation services and programs to individuals recovering from an amputation is a complex process that aims to address the functional, emotional, social and psychological needs of each person.
September 25, 2009 By Anna Kania BSc RMT
An amputation is a physical and psychological trauma that has a profound influence on the daily life of the individual. Providing comprehensive rehabilitation services and programs to individuals recovering from an amputation is a complex process that aims to address the functional, emotional, social and psychological needs of each person.
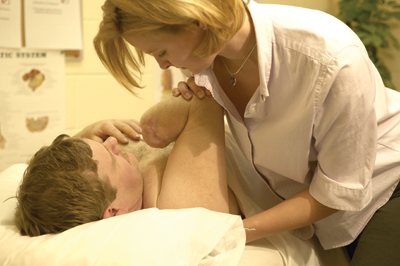 It is generally recognized that in amputee rehabilitation, a multi-disciplinary team approach is required in order to address the individual’s diverse needs. In today’s medical and rehabilitation practice, that team usually consists of a medical doctor, nurse, physical therapist, occupational therapist and psychological support (either psychologist or social worker).
It is generally recognized that in amputee rehabilitation, a multi-disciplinary team approach is required in order to address the individual’s diverse needs. In today’s medical and rehabilitation practice, that team usually consists of a medical doctor, nurse, physical therapist, occupational therapist and psychological support (either psychologist or social worker).
At St. John’s Rehabilitation Hospital, a unique feature of the amputee rehabilitation program is the incorporation of Massage Therapy. Through clinical work and documenting the case by case effects and effectiveness of Massage Therapy in our Massage Clinic at St. John’s Rehabilitation Hospital, a number of benefits of Massage Therapy to the amputee population have become recognized.
OVERVIEWWHAT ARE THE GENERALLY RECOGNIZED BENEFITS OF MASSAGE THERAPY?
The body of research proposing and supporting the effects of Massage Therapy is continuously growing. From this research and literature examining the physical and psychological effects of massage therapy, a list (see Table 1) of generally recognized effects of Massage Therapy has been acknowledged and commonly sited as indicators for referral to Massage Therapy. It is interesting to point out that most of the indicators for Massage Therapy listed in Table 1 are frequently identified as goals of rehabilitation and very relevant to amputee care.
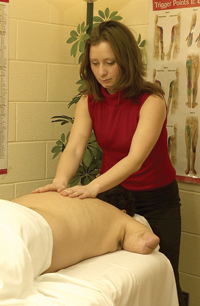 Table 1 – Indicators for Massage Therapy
Table 1 – Indicators for Massage Therapy
• Reduce swelling.
• Increase circulation.
• Reduce muscle tightness and stiffness.
• Reduce scar tissue tightness.
• Reduce spasms.
• Increase muscle length.
• Decrease pain.
• Decrease anxiety and stress.
• Improve sleep (i.e. duration).
• Increase state of relaxation.
MASSAGE THERAPY INTERVENTION FOR TREATMENT OF SYMPTOMS SPECIFIC TO AMUTATIONS
The specific symptomatic picture of an amputee client varies from individual to individual and is also dependent upon the stage of rehabilitation they are in (for example, post-surgery, prosthetic training and/or general maintenance program). Frequently reported symptoms by amputee clients that have resulted in referral for Massage Therapy treatments at St. John’s Rehabilitation Hospital are as follows:
1. PHANTOM LIMB PAIN
Phantom Limb pain is unique to amputee clients. It is the subjective sensation of pain, not arising from an external stimulus, experienced in the part of the limb that is no longer physically present. Research studies suggest that 70-80 per cent (3) of amputees will experience phantom pain. Most report it immediately after surgery, however, studies indicate that 40 per cent may experience significant phantom limb pain after the first year (1). Amputees have described the phantom pain, as burning, stabbing, twisting, cramping, crushing and throbbing.
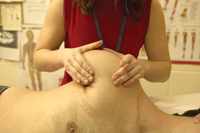 It is frequently sighted in rehabilitation textbooks for amputees that non-invasive techniques such as massage therapy increases sensory input from periphery (the limb) that may over-ride the brains perception of pain which may provide temporary or partial relief of the phantom pain (2). How this is achieved will depend on each individual amputee and the massage therapist’s ability to use their palpation and assessment skills to locate areas where the client reports a change in the pain they are experiencing. Massage treatment may consistent of applying massage directly to the amputated end (the stump), to the muscle and soft tissues above the amputated area (the residual limb) or to soft tissues at the proximal end of the effected limb. A more general massage approach may be appropriate as well, with the goal being to reduce stress and anxiety that are recognized as increasing the intensity or frequency of pain. Reports of massage therapy treatment reducing phantom pain have varying results – that is, for some it has been a great source of relief, where as for others it has had minimal effect. It is, nonetheless, a therapy well worth considering in treatment and management of this very specific type of pain unique to amputee clients.
It is frequently sighted in rehabilitation textbooks for amputees that non-invasive techniques such as massage therapy increases sensory input from periphery (the limb) that may over-ride the brains perception of pain which may provide temporary or partial relief of the phantom pain (2). How this is achieved will depend on each individual amputee and the massage therapist’s ability to use their palpation and assessment skills to locate areas where the client reports a change in the pain they are experiencing. Massage treatment may consistent of applying massage directly to the amputated end (the stump), to the muscle and soft tissues above the amputated area (the residual limb) or to soft tissues at the proximal end of the effected limb. A more general massage approach may be appropriate as well, with the goal being to reduce stress and anxiety that are recognized as increasing the intensity or frequency of pain. Reports of massage therapy treatment reducing phantom pain have varying results – that is, for some it has been a great source of relief, where as for others it has had minimal effect. It is, nonetheless, a therapy well worth considering in treatment and management of this very specific type of pain unique to amputee clients.
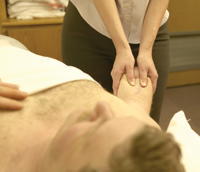 2. RESIDUAL LIMB PAIN
2. RESIDUAL LIMB PAIN
Residual limb is the pain experienced at the distal end of the affected limb that remains after the amputation.
The causes of residual limb pain are numerous, such as: tissue damage during surgery, mechanical factors such as poor prosthetic fit, an unprotected neuroma, rubbing of the skin and joint dysfunctions. Additional factors which may contribute to or be the source of the residual limb pain are referred pain from tight muscles (i.e. trigger points), muscle spasms, adhered scars, poor circulation and swelling. As noted, soft tissues and muscles that are tight, restricted or dysfunctional can be effectively treated with massage therapy, thus providing pain relief to the amputee client (2).
CASE STUDY: Relief of residual limb pain with massage therapy
Mr. X is an out-patient of the Back on Track Program at St. John’s Rehabilitation Hospital. He suffered an accident, which resulted in an upper limb amputation below the elbow. He receives massage therapy three times a week as part of his current rehabilitation program. Mr. X reports a constant burning pain shooting into his residual limb, which he rates to be 9/10 (on the Numerical Pain Rating Scale, where “0” is no pain and “10” is the worst pain) at the beginning of a massage therapy treatment. The 30-minute session includes Swedish techniques and trigger point therapy. The forearm muscles are treated with swedish techniques (petrissage and more localized kneading). Palpatory assessments reveal trigger points in the proximal attachments of the forearm extensors, which were referring pain into the residual end of the amputated limb. After the Massage treatment, Mr. X reports that the pain is 0/10 and this lasts an average of 24 to 36 hours post Massage treatment.
 3. DESENSITIZATION
3. DESENSITIZATION
Many amputees experience sensitive residual limbs or hypersensitivity of the effected limb around scar areas or muscles, which are hypertonic. This often results in a cyclical pattern of increased discomfort and pain that often impedes the use and functionality of the affected limb. Through the direct application of manual techniques to the soft tissues of the residual limb (or stump), massage therapy can be a highly effective method of reducing the sensitivity of the nerves and underlying tissues (muscles, fascia) therefore reducing the associated pain and discomfort (4).
4. MUSCLE TIGHTNESS, STIFFNESS AND SPASMS
Often, amputees will experience pain symptoms in areas that are not directly associated with the amputation. These structures, referred to as compensatory structures, are the muscles and joints that are required to perform new and/or additional functions due to the limitation or inability to perform them with the amputated limb. For example, a right upper extremity amputation results in additional demands being placed on the left arm for lifting and personal hygiene. This imbalance in muscle activity can result in muscular tightness, stiffness, spasms, pain and often leads to the development of repetitive strain disorders in the unaffected limbs. Such factors will further limit the amputees’ functional abilities and should be addressed early in order to prevent or relieve them.
 Here are examples of commonly reported symptoms and syndromes by amputee clients at St. John’s Rehabilitation Hospital resulting from or related to muscular and soft tissue restrictions, tightness or dysfunction:
Here are examples of commonly reported symptoms and syndromes by amputee clients at St. John’s Rehabilitation Hospital resulting from or related to muscular and soft tissue restrictions, tightness or dysfunction:
A. Upper extremity amputees often develop carpal tunnel or related symptoms in the unaffected hand due to increased use and dependence on the unaffected limb to do everything that 2 hand/arms used to do.
B. In lower leg amputees, the weight distribution during standing and walking is often favored to the unaffected limb. Also, alterations in posture and biomechanics in lower leg amputees are very common caused by such things as discomfort at the residual end, muscular weakness of the amputated limb and leg length discrepancies. As a result, lower limb amputees often suffer from persistent low back pain. As was noted by Adeled Fifield, in an article on Back Care in NAC News: “… amputees (both upper and lower limb) are more prone to back pain than the general population” (5).
C. Development of muscle tightness and spasm with the use of prosthetic devices is very common, due to the demands being placed on muscles in performing new activities and carrying the added weight of the prosthetic.
D. Development of contractures in joints above the site of the amputations is a frequent occurrence. As contractures result in lost range of motion of the affected joint, reduction and prevention of contractures is very important in order to avoid complications such as poor prosthetic fit, gait deviations, inability to ambulate with a prosthetic all together, and development of pain in the effected muscles and joints.
E. Headaches are a very common symptom reported by individuals with an amputation. Headaches can be caused by many varying factors such as side effect of medications, poor sleep, stress, dehydration, and muscle tightness. “Trigger points” in muscles of the head, neck and shoulders have common referral patterns of pain into the head and may be the cause of the reported headaches. By decreasing the muscle tightness and related soft tissue restrictions as well as inducing a relaxation effect through massage therapy, headache symptoms can
be managed, if not eliminated.
Assessment to determine the possible cause of the muscular restrictions and reported pain is important in order to develop the appropriate treatment plan. The massage therapy treatment may consist of trigger point therapy, joint mobilizations, and specific massage techniques to the affected soft tissue structures. Postural education and instruction on home care (for example stretching) also becomes a very important component of the Massage treatment.
5. SCAR TISSUE
Many amputees have scar tissue in the affected limb associated with surgery or related to the accident. Scar tissue is tougher, less elastic and often thicker than normal skin and muscle.
Due to its restrictive characteristics, scar tissue can have a negative effect on the neighbouring tissues, resulting in stiffness, pain and limited range of motion. Furthermore, itching and sensitivity of scar tissue is very common, which besides being unpleasant, can reduce the amount of time a prosthetic is tolerated (if it fits over the scar area) or reduced the range of motion of affected joints.
Positive out-comes of scar tissue massage result in reduced tightness, stiffness, pain, itching, an increase in the range of motion of affected and surrounding joints and an overall improvement in movement quality.
6. SWELLING
Swelling (or edema) is commonly experienced by amputees, especially after surgical interventions, elaborate atmospheric pressure changes, and prolonged prosthetic wearing. There are specific techniques that can be applied by the trained Massage Therapist (with specific techniques such as Manual Lymphatic Drainage) that effectively reduces swelling (6).
Reducing swelling is important for tissue health maintenance as well as removing the excess fluid that can compress on internal structures and result in various uncomfortable sensations (such as tingling or numbness) or pain. Furthermore, excess swelling can change or alter a prosthetic fit affecting one’s comfort levels when using the prosthetic and overall functionality, impacting the rehabilitation process in a negative way.
7. INCREASE CIRCULATION
Massage therapy is also recognized for its effect of increasing circulation, systemically and locally (6). Good blood flow and appropriate tissue profusion is very important since it is the source of nutrients and waste elimination to and from all tissues.
Many amputees report poor circulation of the affected limb, which results in a cold, and often times painful residual limb. Winter can be a particularly difficult time as the cold weather reduces peripheral blood flow. Many amputees report it takes a number of hours, if at all, for the residual limb to return to a “normal” temperature and the burning pain to subside. This may be caused by a number of factors: an amputation affects various soft tissue structures that regulate blood flow into the extremities (i.e. nerves and vasodilation/constriction of arteries and capillaries). Another important factor is that after an amputation, muscle atrophy to some degree is inevitable since the muscles are not required to work due to missing hand, leg, etc. The golden rule applies here: “if you don’t use it, you lose it.”
Since muscles that were directly attached to the missing body part have reduced activity and are smaller due to the atrophy, the muscle pump action, which plays a vital role in blood circulation, is missing. Massage therapy can be of great benefit in such situations as the kneading and effleurage strokes can mimic the muscle pump action, thus passively and manually moving fluid in and out the limbs. Furthermore, massage has a direct local effect on increasing the blood to the area that is being treated (often times seen as hyperemia) on the skin surface. Poor circulation can also result in a chronically cold residual limb, which is often correlated with an increased level of pain and phantom pain (2).
Massage therapy can have a short-term or long-term effect in providing relief from the above symptoms. It is important to stress that relief for even a short period of time can have a very positive effect psychologically. A number of studies suggest Massage Therapy to be highly effective in reducing anxiety, stress, and increasing sleep duration (5) – all important factors that have an impact on quality of life, particularly when an individual is involved in a very traumatic accident and is going through an intensive rehabilitation process.
INDICATORS FOR REFERRING TO MASSAGE THERAPY
Massage therapy can be of great benefit to amputees in the various phases of rehabilitation and as a preventative therapy in order to ensure a high quality of life for the amputee client. There are a number of indicators for referral to Massage Therapy.
Incorporating Massage Therapy into a pain management program is highly recommended due to the direct benefit in treatment of soft tissue dysfunction and circulatory problems, and in the positive effect of Massage Therapy on the psychological factors (i.e. stress, anxiety) which may exacerbate the intensity of the pain being experienced.
It is highly recommended that an amputee receive massage therapy in conjunction with the beginning prosthetic training and ongoing prosthetic use in order to prevent muscle strain, tightness and related pain symptoms that may develop due to the alterations in posture and biomechanics.
Prevention of decreased range of motion and development of contractures is a major concern due to the negative impacts on prosthetic fit, inability to ambulate with a prosthetic, and development of pain due to soft tissue and arthritic changes.
The best way to prevent loss of range of motion is to remain active and to ensure that the soft tissues are maintained in a state of good health. Massage therapy intervention is highly beneficial in reducing muscle tightness and stiffness, and maintaining the health of the affected joints.
REFERENCES
- Jeffries, G. Edward. “Pain Management: Post-Amputee Pain.” In Motion; 8 (2). March/April 1998.
- Finsein V., Persen L., Lulien M. “Transcutaneous Electrical Nerve Stimulation after Major Amputation.” J of Bone Jnt Surg (Br). 1988, 70:109-112.
- DiMartino, Christina. “Capturing the Phantom.” 10 (5); Sept/Oct 2000. Available on-line at: www.amputee coalition.org/inmotion/sept_oct_00/phantom.html
- Fifield, A. “Back Care.” NAC News. Vol 2. No. 1. Available on-line: www.waramps.ca/nac/nac2-1.pdf
- Field, Tiffany. “Massage Therapy Effects” American Psychologist. December 1998; 53 (12): 1270-1281.
- Goats, Geoffrey C., “Massage – the scientific basis of an ancient art: part 2. Physiologcal and Therapeutic Effects.” Br J Sp Med. 1994; 28(3): pp 153-156.
- Travell J., Simons D., Simons L. “Myofascial Pain and Dysfunction. The Trigger Point Manual: Volume 1.” Second Edition. Baltimore: Williams and Wilkins; 1999.
Print this page