
Products
Joint Play Mobilization
On May 28, 2008, Lucy (not her real name), a 33-year-old female, came to me seeking relief from achilles pain after hiking. During her interview and discussions, Lucy reported she was also suffering from bilateral de Quervain’s disease (tenosynovitis of the abductor pollicus longus and extensor pollicus brevis), which had been diagnosed by a physiotherapist.
October 21, 2010 By Mike Dixon RMT
On May 28, 2008, Lucy (not her real name), a 33-year-old female, came to me seeking relief from achilles pain after hiking. During her interview and discussions, Lucy reported she was also suffering from bilateral de Quervain’s disease (tenosynovitis of the abductor pollicus longus and extensor pollicus brevis), which had been diagnosed by a physiotherapist.
Her chief complaint was not wrist pain, though, despite the fact that she had been suffering from de Quervain’s debilitating pain for 17 years. She told me not to worry about her wrist pain, as she felt there was nothing to be done about it, and had come to me, anyway, because she had heard that I was good at treating feet and was hopeful that I could help her recover from her achilles pain. In fact, she told me that every time someone worked on her wrist and hand, it would become inflamed and painful. After some convincing, she allowed me to have a look at her wrists. Range of motion in the wrists was markedly reduced on extension and medial and lateral deviation and flexion was also somewhat reduced but, by comparison, not to the same degree. Finklestein tests (tests for de Quervain’s) were positive bilaterally.
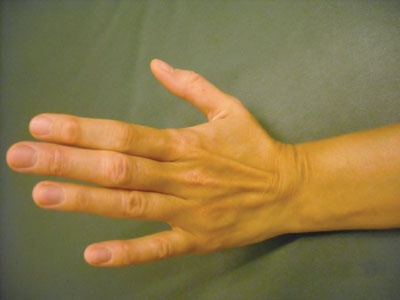 |
|
| Dorsal swelling around capitate bone in the wrist. |
|
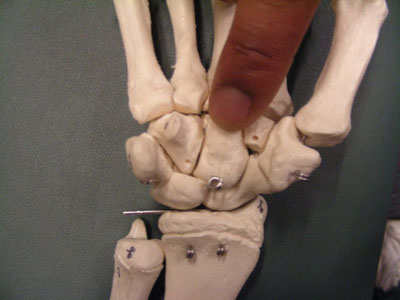 |
|
| Skeletal view of location of capitate bone in the wrist. |
HISTORY AS REPORTED BY LUCY
“At age 16 I started work in a factory, which involved me using a heavy duty tape gun to tape up boxes to be shipped. After repeating this action for a few months my right wrist began to swell and be painful towards the end of the working day. The pain seemed to stem from the joint at the base of the thumb and the whole wrist would swell and I would have very limited movement. I visited my local GP who advised me that I had tendinitis and I should strap my wrist and try not to use it. I started to use my left wrist to perform my job. It was quite awkward but I got used to it and after a while the same symptoms appeared in the left wrist.
“Over the years, I avoided, or tried to limit, the things which upset my wrists, but because of this, both wrists became very weak and movement was always limited. Even without pain or swelling, my wrists would only extend to a 30-degree angle.
“For 17 years my choices had been dictated by my wrists until I was recommended to visit Mike Dixon by his co-worker Mark. Mike said my scaphoid bone was stuck, which was causing the tendon to get inflamed, resulting in swelling and discomfort. Mike manoeuvred the scaphoid bone so it was no longer pushing on the tendon.
“Since then I have been using my wrists without pain or swelling, I am able to type and write, prepare food and stir sauces, all the things I used to try and avoid, I am now able to do without pain or swelling.”
WHY DID HER CONDITION RESOLVE?
I believe that Lucy had subluxations of a few of the carpal bones. These subluxations changed the biomechanics of the wrist and hand and led to an unresolving somatic dysfunction. A somatic dysfunction is an “impaired or altered function of related components of the somatic (body framework) system; skeletal, arthrodial, and myofascial structures; and related vascular, lymphatic, and neural elements.”1
Simply put, when a joint becomes dysfunctional, all tissues associated with that structure also become dysfunctional. This means the joint capsule, any muscles involved in moving the joint, fascia support, and connecting structures, such as nerves, blood vessels and lymphatics, all become affected. This leads to that pain-tension cycle that is unresolvable until alignment is restored and the body can begin the healing process.
So, in “Lucy’s” case, there were three elements to be addressed in order to restore function to her wrists.
The first was her capitate. I found it to be subluxed anteriorly, which disrupted the movement of all the carpal bones; second, her scaphoid was reduced in its joint play anteriorly, medially and laterally; and third, the trapezium had become hypermobile to accommodate the hypomobility of the scaphoid. This led to the irritation of the thumb, outcropping tendons and thus the condition of de Quervain’s. This begs the question of whether it was really de Quervain’s or merely a somatic dysfunction of the carpals disguising itself as such. I believe the latter is true, but this is only speculation. What is significant to the scope of this article is that the condition has resolved and she can now enjoy full use of her hands.
THE BIOMECHANICS OF THE WRIST COMPLEX
Arthrokinetics
For the most part, extension of the wrist occurs at the proximal radiocarpal joint, while flexion is primarily at the mid-carpal joint. Most of the gliding joint surfaces follow a convex-on-concave arrangement. This means that the roll and glides occur in opposite directions. There are two exceptions to this in the wrist. They are the trapezium (under the thumb) and the trapezoid (just proximal to the second metacarpal). These two carpals have concave articulations that glide on the distal-radial portion of the scaphoid. Thus these two bones follow the concave-on-convex rule, which is to roll and glide in the same direction. In other words, when you move your wrist into flexion, most of the carpals move anteriorly (toward the palm) and, conversely, they move dorsally when the wrist moves into extension, with the two exceptions of the trapezium and trapezoid.
This articular arrangement makes us subject to anterior displacements of the carpal bones when we load or compress into extension. This explains why a “Foosh” (falling on an outstretched hand) type injury causes palmar subluxations of the carpals. The lunate is especially prone to dislodge into the carpal tunnel. (This is one of the causes of carpal tunnel syndrome.) One of the carpal bones that is largely overlooked, in my opinion, is the capitate, which may also be subluxed or moved towards the palm. It forms a large portion of the floor of the carpal tunnel and can, therefore, compress the structures travelling through this tightly controlled tunnel.
Mobilization of the Wrist and Hand Complex
In my practice and in my teaching, I have the opportunity to practise mobilizations of the wrist and hand complex almost daily. Students, staff and patients alike often suffer with wrist pain from displacement of carpals, as discussed above. I am very often called upon to perform these mobilizations of the capitate, trapezoid, scaphoid, and lunate with my colleagues, friends, family and, yes, sometimes students.
Massage therapists, due to the nature of their work, have their hands in extension for prolonged periods of time. Effleurage is a good example of having the wrist move into extension, particularly at the beginning of the stroke. This puts the wrist into a position of compromise. You may be surprised at how much pressure is being applied to the wrist during an effleurage technique. If you are a massage therapist – and likely you are if you are reading this article – do yourself a favour and get the bathroom scale: do a pressure check to see how much pressure you typically use to do an effleurage – you may find it impressive.
When the wrist is placed into extension and pressure is applied, the carpal bones move towards the palm. The capitate, which is the largest of the carpal bones, can become subluxed towards the carpal tunnel. This causes the capitate to lose its dorsal glide, resulting in the wrist becoming dysfunctional. Another contributing factor may be the fact that the adductor pollicus muscle has an anterior attachment to the capitate. If we (massage therapists) use our thumbs too much, the adductor can become overused. This muscle, because of its carpal attachment, may contribute to the anterior displacement of the capitate. Very simply, if you release the adductor pollicus muscle with digital pressure, and stretch, then mobilize the capitate posteriorly, followed by assessing and mobilizing the scaphoid (palmarly, dorsally or both), these techniques can go a long way in reducing the somatic dysfunctions associated with these very common biomechanical disruptions.2
SO, WHAT ARE THE BENEFITS OF JOINT PLAY MOBILIZATIONS?
Benefits of these techniques include restoring the joint alignment and glide component motions. These were invaluable in Lucy’s case, but also in a plethora of other cases I have seen over the years. Joint play mobilizations not only restore gliding component motions within the joint structures, but also help to rehydrate joints, reduce pain, reduce muscle spasms, and increase range of motion. Most importantly, they may help improve overall function and, therefore, overall health. With proper training, joint play mobilizations are easy to perform, and prove over and over again to be well worth the added effort it takes to understand joint structures and the interrelationship these tissues play (no pun intended) with the overall human body.
THOUGHTS ON TREATING SOMATIC DYSFUNCTION
If the dysfunction affects all levels of tissues, such as described earlier, then does it not make sense to treat all levels of dysfunction, as all tissues affect all other layers of tissues in the somatic zone? If the skin is sore, treat the skin; if the muscles are sore, treat the muscles; if the fascia is restricted, treat the fascia. If the joint is reduced in its range of motion, it just makes sense to treat the joint. Joint play is one way to do this effectively. If you are not sure how to affect the glides, try distracting the surfaces apart, as this is sometimes enough to reduce a subluxation, and /or an articular dysfunction, thus improving range of motion and decreasing pain. I find the outcomes tend to be improved when massage is combined with stretching, muscle energy, joint glide manipulation and nerve mobilizations. This multidimensional approach allows treatment of all levels of the dysfunction.
UTILIZATION OF JOINT PLAY TECHNIQUES
“Joint manipulation is an ancient art and science that can trace its origins to the earliest medical and lay practitioners. Today, it is practiced principally by physical therapists and chiropractors and to a lesser degree, by osteopathic and medical physicians. Self-manipulation of both joint and soft tissues is also a common practice in those who “crack” their own knuckles and spines.” 3
As you can see from the above quotation, massage therapists are not mentioned. However, it is my opinion that massage therapists should utilize these techniques as well, in order to achieve improved patient outcomes and to stand tall next to other health-care providers. The question is, do we? We learn these techniques in undergraduate studies, and then they are typically displaced by the enormous amount of information required to pass board exams. We are, however, an evolving therapy and many therapists are achieving marvellous results. What I strongly suggest is that you attempt to evolve joint play techniques into your practice – you may be surprised by the results.
What I love about massage therapy is the terrific outcomes that we all can achieve.
REFERENCES
- Principles of Manual Medicine, Second Edition, by Philip E. Greenman.
- Joint Play the Right Way for the Peripheral Skeleton. Third Edition. 2009, by Mike Dixon.
- A history of manipulative therapy through the ages and up to the current controversy in the United States, by Paris Stanley, Journal of Manual & Manipulative Therapy, Volume 8, Number 2, 2000, pp. 66-77(12).
BIBLIOGRAPHY
- Carolyn Kisner, MS, PT, and Lynn Allen Colby, MS, PT. Therapeutic Exercise, Fourth Edition, 2002.
- Cynthia C. Norkin, EdD, PT, and D. Joyce White, DSc, PT. Measurement of Joint Motion: A Guide to Goniometry, Third Edition, 2003.
- Darlene Hertling, BS, RPT, Randolph M. Kessler, MD. Management of Common Musculoskeletal Disorders, Physical Therapy, Principles and Methods, Second and Third Editions, 1996.
- Darryl Lajeunesse, Carol Edwards and Brenda Grosenick. Realism, A Study in Human Structural Anatomy, 2003.
- David J. Magee, PhD, BPT. Orthopedic Physical Assessment, Second and Third Editions, 1996.
- Disorders, Physical Therapy, Principles and Methods, Second and Third Editions, 1996.
- Frank H. Netter, MD. Atlas of Human Anatomy 1993, The CIBA Collection of Medical Illustrations, 1991.
- Janet G. Travell, MD, David G. Simons, MD. Myofascial Pain and Dysfunction, The Trigger Point Manual, Volumes 1 and 2, 1992.
- Joseph E. Muscolino. The Muscular System Manual – The Skeletal Muscles of the Human Body, 2005.
- I.A. Kapandji. The Physiology of the Joints, 1970.
- Joseph E. Muscolino. Kinesiology: The Skeletal System and Muscle Function.
- Laura K. Smith, Elizabeth L. Weiss, L. Don Lehmkuhl. Brunnstrom’s Clinical Kinesiologly, 5th
- edition, 1983.
- Nikita A. Vizniak, DC. Clinical Consultant Physical Assessment, 2nd Edition: 2005.
- Pamela K. Levangie, Cynthis C. Norkin. Joint Structure and Function: A Comprehensive Analysis, Third Edition, 2001.
- Philip E. Greenman. Priniciples of Manual Medicine, Second Edition.
- Rene Cailliet, MD. Soft Tissue Pain and Disability, 9th printing, 1985.
- Robert B. Salter, MD. Textbook of Disorders and Injuries of the Musculoskeletal System.
- Robert E. McAtee. Facilitated Stretching, 1993.
- Stanley Hoppenfeld, MD. Physical Examination of the Spine & Extremities, 1976.
- Steve Anderson, RMT, BSc. Anatomy and Kinesiology lecture notes, 1992.
- Susan L. Edmond, MPH, PT. Manipulation Mobilization and Spinal Techniques.
Mike Dixon has practised massage therapy for 25 years. He is an educator, a published author, and an international presenter in massage therapy continuing education (Arthrokinetic Therapy). Mike graduated from the West Coast College of Massage Therapy in 1986 and has been teaching at the school since 1993.
Mike was also the senior practical advisor for the college. His specialty is in orthopedics assessment and treatments. He also teaches at the Boucher Institute of Naturopathic Medicine.
Print this page