
Features
Continuing Education
Education
Journal highlights progress in lymphedema care after cancer treatment
Individuals who have been treated for cancer are at risk for a complication called lymphedema: swelling in the body region where lymph nodes were removed, causing pain and limited function. New research and insights on the management of cancer-related lymphedema are presented in the January special issue of Rehabilitation Oncology, official journal of the Oncology Section of the American Physical Therapy Association. The journal is published by Wolters Kluwer.
January 23, 2018 By Newswise
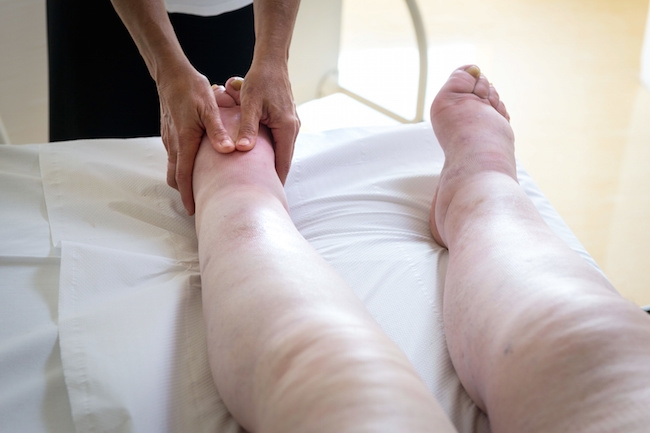
The special issue highlights progress in rehabilitation and physical therapy management of cancer-related lymphedema – including a new study identifying characteristics of patients who need extra support in practicing essential self-care. Other articles point toward ongoing advances in lymphedema care, including new imaging techniques, and technologies to help patients monitor and control their condition, according to an introduction by guest editor Nicole L. Stout.
Lymphedema is a complication of cancer treatment that occurs due to fluid buildup in soft tissue, resulting from damage to the lymphatic system. Patients with lymphedema experience painful swelling and limitation of function of the limbs or other areas.
Complex decongestive therapy (CDT) is the multimodal treatment for lymphedema carried out by a skilled therapist. However, in order to optimally manage the condition, some components of CDT need to be carried out by the patient on a daily basis. Self-care plays an important role for patients with lymphedema, and may include daily self-massage, skin care, compression therapy and exercise. However, for some individuals with lymphedema, performing daily self-care poses a challenge.
Dr. Helene Lindquist, Tommy Nyberg and their research group at Karolinska Institute, Stockholm, performed a study to identify characteristics of women who needed extra support to self-manage their lymphedema. The study included data on 88 Swedish women, average age 62 years – most with arm lymphedema after breast cancer treatment.
Nearly 60 per cent of women in the study performed their self-care program almost every day – even though about half of the patients felt that self-care did not help much. Only about 20 per cent of women who worked performed daily self-care at work.
A wide range of demographic, clinical, psychological and physical characteristics were significantly related to self-care practice. Factors associated with lower rates of daily self-care included low scores for well-being, body image and self-esteem; ethnicity other than Swedish; depressed or anxious mood; and poor sleep quality.
“Our results emphasize the importance of focusing more on vulnerable individuals when it comes to instructions about self-care and to encourage women to perform continuous self-care,” the researchers write. They believe their findings support a “stepped-care” approach to working with women with lymphedema: basic help for all women, with stepwise progressive interventions for those in need of additional support. The special issue includes a narrative by actress Kathy Bates – a breast cancer survivor with lymphedema – providing a patient’s perspective on the frustrations and arduous nature of the ongoing self-care needs.
Stout notes the special issue appears two decades after a seminal report by the American Cancer Society on lymphedema management. Since then, management of lymphedema has become “far more mainstream,” with ongoing research, clinical practice guidelines, and improved access to specialist care. Other topics in the special issue include patient assessment, considerations for advanced training for physical therapy professionals in lymphedema care, and new imaging approaches.
Other papers report on sophisticated technologies like low-level laser therapy. These advances open the possibility of developing wearable sensors and cloud-based apps to provide patients with daily feedback on their condition and individualized updates for support and prevention. Stout concludes, “The future is bright, the future is smart, and we must continue to seize on opportunities to advance novel approaches to lymphedema management.”
Print this page