Features
Practice
Technique
Lower limb referral: Pain we can understand
January 25, 2022 By Caleb Fenton, RMT
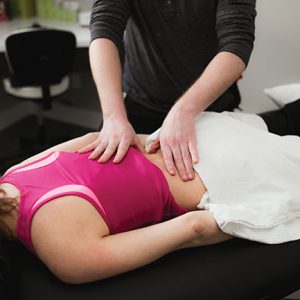
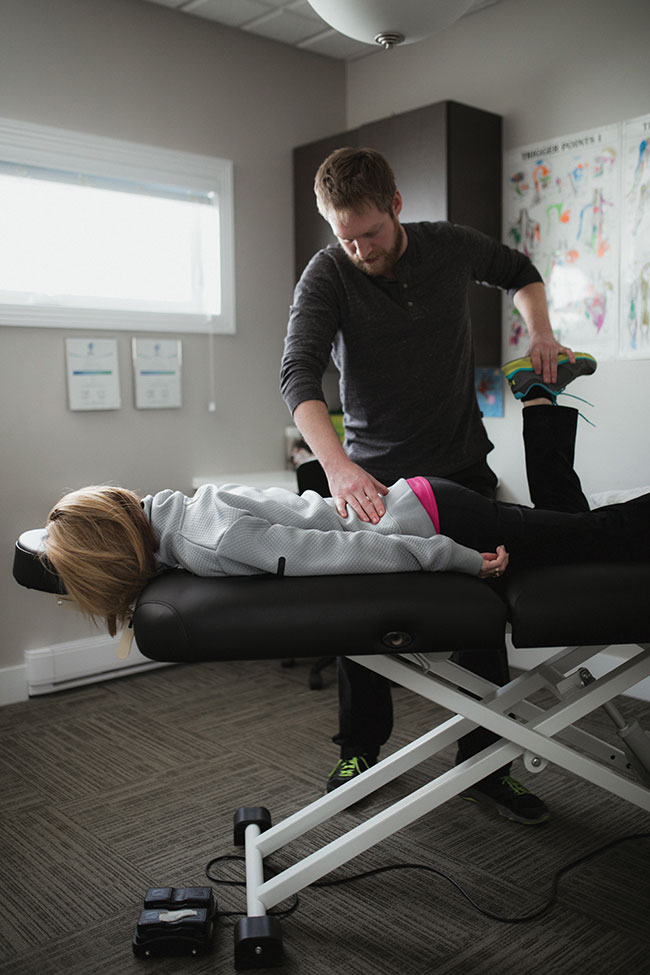 Hibb’s Special test - examination for Sacroiliac dysfunction. Can also aid in ruling in piriformis syndrome.
Photos: awaken collective - David Bryan photography
Hibb’s Special test - examination for Sacroiliac dysfunction. Can also aid in ruling in piriformis syndrome.
Photos: awaken collective - David Bryan photography When a discomfort begins to radiate, then we can begin to narrow down root causes. It’s simpler because neurological referral patterns have a distinct pathway with blanketed type symptoms; Burning, shooting or zapping/electric type pain with numbness and tingling, and often weakness experienced in the lower limb.
In this article I want to cover a small handful of referral type patterns into the lower limb, building from the more “local” type discomfort in the lower back.
Facet injuries and referrals
The anatomy of the facet is the posterior interlocking articulations of the lumbar spine. With a superior articular facet of the lower lumbar vertebra joining to the inferior articular facet of the superior lumbar vertebra, we establish a joint and its capsule that when either vertebra moves, the adjoined vertebra reacts and moves with its “locked” superior and inferior vertebra. The orientation of the facet in the lumbar spine is roughly 90° in the saggital plane. Allowing ONLY flexion and extension of the lumbar spine. With rotation and lateral flexion, each vertebra needs to partially flex, then rotate to establish a mild movement. This is often the cause – we will treat many lower back injuries resulting from regular rotation, especially with a load.
Facet irritations are commonly a local discomfort. A feeling of a deep dull, aching sensation, with a pinching type discomfort when the facet is placed in a “closed-packed” position. They may vocalize hesitations with flexion of the trunk, or use the term “I threw my back out,” when lifting something heavy. Yes, this also indicates a sprain/strain injury as well, however, due to the lack of instability of the ligaments and muscles, this can increase the chances of load on the joints. Furthermore, there may be a “joint referral,” a type of diffuse discomfort with no sensory or muscular pattern.1 It’s a type of discomfort that does NOT radiate past the knee, rather more into the buttock and into the thigh.2 Causes of referral are unknown, mainly it does not follow a typical radicular pattern into the lower extremities.
A typical provocation factor of facet irritation may be that as the day progresses and with a prolonged load on the spine (this comes from standing or sitting for prolonged periods) the discomfort worsens, laying down can alleviate the symptoms. This would indicate that your patient may experience more discomfort at the end of the day and need to sit and rest especially in a reclined position.
Hip bursitis and referrals
Bursae are synovial fluid-filled sacs, that act as buffers between the bone and the tendons of a muscle, creating a cushion and increased viscosity. As the muscle pulls the bone into movement, there is a gentle glide, almost eliminating bone-to-muscle friction. Specific to the hip we’ll briefly cover greater trochanter, iliopsoas and ischiogluteal bursitis.
 Often through direct or blunt trauma, resulting from contact sports, infection via diabetes, repetitive strain and overuse to the muscles near the bursa or prolonged compression injury, the bursa can become irritated or inflamed, causing pain and tenderness over the location. Increased activity can also further aggravate the bursa.
Often through direct or blunt trauma, resulting from contact sports, infection via diabetes, repetitive strain and overuse to the muscles near the bursa or prolonged compression injury, the bursa can become irritated or inflamed, causing pain and tenderness over the location. Increased activity can also further aggravate the bursa.
To begin, the bursa located at the greater trochanter, often has pain and tenderness with palpation at the greater trochanter and the lateral aspect of the thigh, following the IT band and not crossing the knee.3 The client may experience burning along the lateral thigh, mimicking meralgia paraesthetica.4 Difference is no paraesthesia or hyperesthesia is present as peripheral neuropathy. Clients will have difficulty laying on the affected side and in some extreme cases, will have difficulty wearing tight or more fitted pants. Symptoms worsen with activity like walking, jogging or jumping – essentially any activity that includes repetitive hip flexion and extension.
Iliopsoas bursitis (IPB), a part of the true hip pain region, is located proximal and medial aspect of the coxa and posterior to the iliopsoas tendon. IBP has a diffuse, achy and burning sensation at the inguinal region, groin and proximal anterior thigh. The referral pattern follows the femoral nerve. Tendonopathy of the iliopsoas muscle would also be present. Flexion and adduction of the hip would be difficult, weak in fact due to pain or a pinching distal to the inguinal region, but no weakness with knee extension differentiating from femoral nerve entrapment.
Finally, ischiogluteal bursitis (IGB), also known as weaver or tailor bottom,5 is located at the ischial tuberosity of the ilium, which is near the gluteal fold. A staple symptom of IGB, the client will share that it feels like they are sitting on a marble or the belt buckle in the car. There is tenderness with palpation over the tuberosity and worsens when you request the client to flex their knee with resistance. Having a sedentary lifestyle places individuals at risk, and that risk increases when they sit for prolonged periods on hard surfaces, hence the rare instance of mechanical injury.
Nerve root impingement referrals
Nerve root impingement is the “poster child” in many conventional therapies with regards to radiculopathies. The staple signs and symptoms include: weakness or rapid fatiguing; numbness and tingling (paraesthesia); shooting, electric or zapping type discomfort. With prolonged or severe lesions we can visually see tissue atrophy, decreased skin elasticity and loss of complexion.
Nerve root impingement is commonly assumed a disc herniation or “bulge,” where the nucleus pulposus leaks or presses through the annulus fibrosis tissue, due to weakness from degeneration or trauma.
This is a partial truth, albeit the most common cause. However, stenosis of the intervertebral foramen is causing the nerve root impingement. Degenerative changes (spondylosis)6 of the spine can cause narrowing of the foramen, as well as spurs and a change in the vertebra orientation (spondylolisthesis),7 or swelling of the facet joint (hypertrophy), tumours or benign growths. Disc herniations do cause stenosis, but I want to challenge you, it’s not the “only” cause.
Two important notes, lumbar nerve root impingement will ALWAYS cause a referral pattern and/or pain that will cross the knee and secondly, often can resolve on their own.8 The absolute loss of sensation or motor function is a complete rupture or tear of the nerve.
Discussing all causes and patterns of nerve root impingement is an article in itself. However, I want to cover something basic. Nerve root impingement caused by a disc will have increased pain in the mornings due to the hydration, known as imbibition of the discs when we are resting. This will result in increased pressure on the annulus fibrosis causing the nerve to become more irritated when upright. Likewise, nerve root discomfort resulting from facet hypertrophy will present with increased symptoms later in the day. As the disc shrinks, this can place increased stress and overload on the facet joints, increasing the inflammatory response of the capsule.
So, nerve root impingement can have similar symptoms, but a different cause. It’s the intuitive nature of therapists through study to aid in identifying the root issue so we can better approach treatment styles.
Peripheral neuropathies
Finally, peripheral neuropathies, specifically in the lower limb, will often have signs and symptoms that mimic nerve root compression, with a very specific difference: often these injuries are classified as mononeuropathies. (Basically, an injury to a single nerve.) Nerve root injuries can affect multiple nerves, peripheral nerve injuries can often affect only one nerve. An example of this would be tibial nerve compression (tarsal tunnel syndrome) or lateral femoral cutaneous nerve compression (meralgia paresthetica). With these peripheral neuropathies, we have a specific location of compression or lesion.
However, an important note to remember, neuropathies will ALWAYS have symptoms DISTAL to the injury site. So knowing this, the more proximal the symptoms, the higher the lesion. This can further complicate symptoms. As we begin to come closer to the spine, the vastness of nerve bundles increase, thus creating more multiple mononeuropathies.
So what are some common causes of peripheral neuropathies? Trauma is one, whether it be direct blunt trauma, overstretching or a laceration. Other causes include injury from diabetes and unfortunately, roughly 50% of those that are treated with chemotherapy.9 Thanks to research we can also classify neurological conditions in three categories (much like sprain/strain injuries): Neuropraxia, axonotmesis, neurotmesis. These classifications are known as the seddon classifications.10 These classifications help us further understand the prognosis of peripheral neuropathies. This is important because it can help us with the direction of treatment. Are we trying to reduce symptoms and conventional therapies aid? Or, are we wanting to maintain symptoms and try to decrease pain and compensations?
Neuropraxia is commonly known as a stinger – a crush injury where the recovery can take as little as 12 hours, to six to eight weeks for full recovery.
Axonotmesis is a greater stretching or crush injury. The outer sheath of the nerve is still intact, however the axon has been ruptured. Healing is still probable, some studies indicate 1-inch per month. Complete recovery can take six to 12 months.
Neurotmesis is the complete rupture of the axon, myeline and it’s sheath. Some recovery is possible, but complete is impossible and surgical intervention is necessary. Neurotmesis will often result from chemotherapy or prolonged ischemia.
Furthering our understanding and knowledge to pain and radiculopathy, very much aides in greater clinical outcomes, or at least provides us with a means to communicate with our clients what may be the cause to their symptoms, after we have assessed and researched ourselves. We might not be able to give our clients 100% relief, but what we can do is provide our clients the necessary information and referring our clients to the appropriate professionals. We can partner together and hopefully give our clients the relief they are looking for.
References:
- Facet Joint Pain. Seattle Physcial Therapy. May 3, 2018. https://www.unionpt.com/facet-joint-pain-seattle-physical-therapy/
- Facet Joint Syndrome/Arthritis. Mayfield Brain & Spine. Reviewed by; Robert Whitten MD, Marc Orland MD. Sept. 2018 https://www.mayfieldclinic.com/pe-facet.htm
- Aaron J. Seidman, Matthew Varacallo. Trochanteric Burisits. July 18, 2021. https://www.ncbi.nlm.nih.gov/books/NBK538503/
- Physiopedia. Meralgia Paraesthertica. https://www.physio-pedia.com/Meralgia_Paraesthetica
- Johnson DB, Varacallo M. Ischial Bursitis. InStatPearls [Internet] 2019 Mar 19. StatPearls Publishing.
- Kimberley Middleton, David E. Fish. Lumbar spondylosis: Clinical presentation and treatment approaches. March 25, 2009. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2697338/
- Steven Tenny, Christopher C. Gillis. Spondylolisthesis July 25, 2021. https://www.ncbi.nlm.nih.gov/books/NBK430767/
- Coster S, De Bruijn SF, Tavy DL. Diagnostic value of history, physical examination and needle electromyography in diagnosing lumbosacral radiculopathy. Journal of neurology. 2010 Mar 1;257(3):332-7.
- Renata Zajaczkowska, Magdalena Kocot-Kepska, Wojciech Leppert, Anna Wrzosek, Joanna Mika and Jerzy Wordliczek. Mechanisms of Chemotherapy-Induced Peripheral Neuropathy. March 22, 2019. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6471666/
- Avneesh Chhabra, Shivani Ahlawat, Allan Belzberg, Gustav Andreseik. Peripheral nerve injury grading simplified on MR neurography: As referenced to Seddon and Sunderland classification. July-Sept 2014.://www.ncbi.nlm.nih.gov/pmc/articles/PMC4126136/
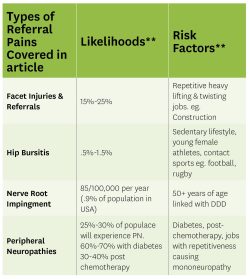
**information based on a collaboration of studies. Each studied indicated different percentages and risk factors.
CALEB FENTON, RMT, SMT (cc) has been a massage therapist for nine years and graduated from the Professional Institute of Massage Therapy with honors. He currently practices in a busy multiple disciplinary clinic with other RMTs, physiotherapists and chiropractors in Steinbach, Man
Print this page