
Features
Practice
Rehab for new moms: The RMT role in promoting pelvic health for postpartum patients
When you ask most massage therapists if they offer postpartum massage therapy, they usually answer quickly in the affirmative. Most of us are aware of the obvious presentations that follow giving birth such as extreme fatigue, back pain, edema, emotional fluctuations, etc.
January 15, 2019 By Michelle Francis-Smith and Nicole Nifo
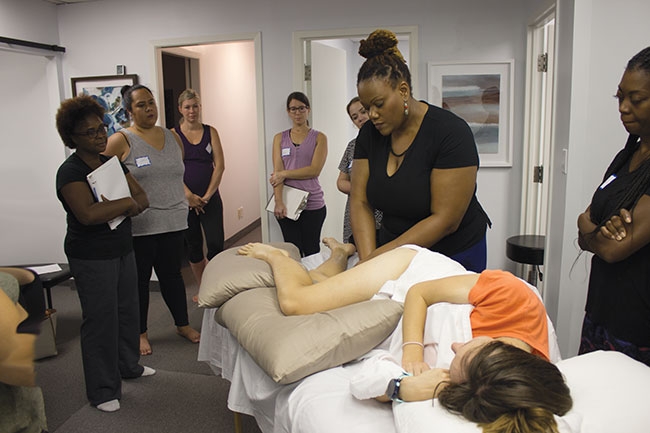 Providing postpartum massage therapy goes far beyond laying hands on a person who has given birth
Providing postpartum massage therapy goes far beyond laying hands on a person who has given birth While those presentations are very common and often reported to us by our patients, there are other impacts that often go unspoken and therefore, untreated. One significantly impacted area for someone who has given birth is the pelvic floor. We believe providing postpartum massage therapy goes far beyond laying hands on a person who has given birth, into providing postpartum rehabilitation and education not always accessible to most of the public.
Pelvic health
The pelvic floor (PF) is a collection of muscles, nerves, tendons, blood vessels, ligaments and connective tissue interwoven in the pelvis. It extends from the pubic bone to the coccyx and the ischial tuberosities. During respiration it lowers and rises in synergy with the diaphragm.
The muscles of the pelvic floor consist of the pelvic diaphragm (levator ani muscle and coccygeus muscle), urogenital diaphragm (deep transverse perineal, sphincter urethrae), and the sphincters and erectile muscles of the urogenital and intestinal tract (external anal sphincter, bulbospongiosus, ischiocavernosus, superficial transverse perineal).
The main function of the PF is to support internal organs (uterus, bladder, large intestine), the sphincter to maintain continence, sexual role, stability and control of the pelvis and spine, and sump-pump action through respiration. During pregnancy the uterus grows more than five times its original size and the load on the PF increases significantly, often causing symptoms of pain and altered function. There is an even greater load during the pushing phase of labour. In order for a full and accurate assessment of the PF, postpartum patients should see a pelvic floor physiotherapist who is able to access these structures internally and diagnose any dysfunctions that might exist. While it is not in our scope of practice to treat internal structures, we do have access externally to the musculature of key target areas. It is helpful for our work and to our patients to understand the role of pelvic floor physiotherapists and be able to offer a collaborative approach to care. “Working in collaboration has been a large benefit to patient care – especially continuity of care, when physios and RMTs work in the same clinic,” says Laura Apps, physiotherapist and owner of Women’s Health Physiotherapy Centre in Ajax, Ont.
“Most pelvic clients come to physiotherapy with many comorbidities. There is almost always external tension and an up regulated nervous system in a women who is seeking care for pelvic pain,” she says. “Having a trusted massage therapist to tackle the external drivers allows us to treat with greater success internally.”
Collaborating with physiotherapists who specialize in pelvic floor treatments provides a quicker recovery and return to optimal function of postpartum massage patients.
Postpartum cases
Patient #1 – Six weeks postpartum, post cesarean section, experiencing mild numbness over her scar, increased muscle resting tension in upper and lower back and gluteals.
Patient #2 – One-year postpartum, vaginal delivery, lower back pain and dyspareunia (painful intercourse), increased muscle resting tension in lower back, gluteals and adductors.
Patient #3 – Eight weeks postpartum, previously an active runner. Obstetrician has given the approval to return to running. Patient is experiencing leakage of urine and general tightness in the hip flexors and quadricep muscles.
Best practices and recommendations
Always position your patient for safety and comfort. If a patient is post-vaginal delivery, all positions can be utilized based on preference. Avoid prolonged prone positioning immediately following delivery when core muscles are likely to be weakened. If a patient is post-cesarean delivery, prone positioning should be avoided for four to six weeks postpartum, or until the scar is unionized and the patient has no discomfort lying on their stomach. It is ideal to treat in side-lying, as there will likely be breast tenderness due to breast tissue changes from lactation.
We have developed a general protocol for how we treat our postpartum patients to address the PF. Using the three patient examples above, our approach remains the same. For the first few massage sessions, the goal is always to assess, palpate and treat the following target areas:
- Lumbar musculature (erectors, multifidus, quadratus lumborum, latissimus dorsi)
- Gluteal musculature (maximus, medius, minimus, piriformis, obturator internus, gemellus superior and inferior, quadratus femoris)
- Inner thigh (adductor minimus and magnus, obturator externus, pectineus, gracilis )
- Hip flexors (TFL, quadriceps, sartorius)
- Abdomen (rectus abdominis, external and internal obliques, psoas, iliacus)
Self-care for patients
Some massage therapists may find it difficult to motivate their postpartum patient to practice self-care due to the overwhelming demands that parenting has on their daily routine. It’s important to keep any self-care recommendations for these patients simple and easy to implement.
According to Boyle et al., incontinent postnatal women who received pelvic floor muscle training (PFMT) were less likely to report urinary incontinence 12 months after delivery. And for women who are continent during pregnancy, PFMT may prevent urinary incontinence up to six months after delivery.
Teaching a simple “core breath” to your patient can be an easy way to create awareness of their pelvic floor and of their posture.
According to educator and physiotherapist Julie Weibe, pelvic stability is maintained through an internal pressure system of the pelvic floor and diaphragm, which she describes as a “piston” that must work together synergistically.
The pelvic stability is provided by the relative maintenance of intra-abdominal pressure by the dynamic relationship between the diaphragm, pelvic floor (PF) and transversus abdominis (TA) muscle. When we take a breath in, the diaphragm contracts and descends, the TA opens, the PF lowers to accept the abdominal contents. When we exhale, the TA and PF (which have been stretched out/elastic loading during inhalation like a rubber band) snap back into place to create stability again and brings the abdominal contents back up while the diaphragm recoils.
When teaching your patient to breathe and perform a kegel (better known as a core breath), it is important to cue them as follows: Inhale to expand the pelvic floor and exhale to engage (or pick up a blueberry). Proper alignment is crucial when teaching your patient this type of core breathing. Doing a thorough postural assessment will help you to cue your patient on better standing and seated posture while engaging the pelvic floor.
Treatment planning for patients with a vaginal versus cesarean delivery
It is a great misconception among patients that those who have had a cesarean delivery will be free from pelvic floor dysfunction when compared to someone who has had a vaginal delivery. According to a study published by Almeida EC, et al. in the International Journal of Gynecology & Obstetrics (2002), in women with chronic pelvic pain, a history of cesarean section was observed at 67.2 per cent of cases.
For this reason, we suggest patients who have given birth in both cesarean and vaginal deliveries be assessed by a pelvic physiotherapist and given a pelvic floor rehabilitation program. Patients who have experienced a cesarean delivery should also be on a treatment plan to rehabilitate the scar.
Massage therapists are already equipped with the knowledge to treat the target areas most affected when pelvic floor dysfunction exists. By using the recommended guideline we have found that we can have a positive impact on reducing symptoms relating to pelvic floor dysfunction and improve the quality of our patient’s lives.
Michelle (B.A., RMT) and Nicole (RMT) are the co-founders of Perinatal Massage Therapy Education. They inspire to empower and educate massage therapists with tools to more effectively and confidently work with perinatal patients. They provide continuing education courses in pregnancy, postpartum and infant massage, to help build your toolkit and increase your confidence to transform your perinatal massage practice and business. pregnancymassagetherapy.com
Print this page