
Features
Practice
Technique
Is craniosacral therapy an appropriate modality for concussion and post-concussion syndrome?
The use of the terms “concussion” and “post-concussion” syndrome (PCS) has increased in the lexicon of health-care practitioners and laypeople. In minor league, amateur and professional sports, we see an increased frequency in the diagnosis of concussion injury as well as the detailed quantification of its accompanying signs and symptoms.
November 2, 2011 By Yonina Chernick
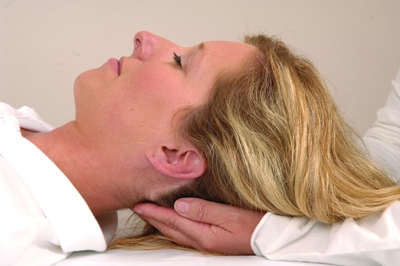
The use of the terms “concussion” and “post-concussion” syndrome (PCS) has increased in the lexicon of health-care practitioners and laypeople. In minor league, amateur and professional sports, we see an increased frequency in the diagnosis of concussion injury as well as the detailed quantification of its accompanying signs and symptoms.
PCS has arisen as the term used to describe the unresolved chronic continuation of a group of physical, emotional and cognitive symptoms. In contrast to the usual seven- to 10-day resolution for sports-related concussions, or up to three months for non-sports-related concussions, the aforementioned symptoms may be reported for months, or even years, after the injury.1
Sign up to get the latest news and events from Massage Therapy Canada
Estimates of the incidence of PCS range from seven per cent up to 33 per cent of patients diagnosed with concussion2,3 and finding treatment approaches to help athletes and laypeople alike has been a challenge for all areas of medical practice. As clarification of the mechanisms of injury and the structures involved continues to develop, employing a manual technique capable of accessing and addressing the vascular, structural and neurological tissues of the brain has surfaced as being an appropriate treatment modality. In particular, the techniques of craniosacral therapy, a gentle and precise osteopathic technique, can be applied with the intention of addressing three main areas of consideration in this type of injury: the cerebrospinal fluid and venous sinus systems; the cranial bones and attached intracranial membrane system; and the autonomic nervous system.
HISTORY OF CRANIOSACRAL THERAPY
Craniosacral therapy has its origins in osteopathic medicine. In the 1890s, a general practitioner, Dr. Andrew Taylor Still, practising medicine in the midwestern United States, faced a family crisis of meningitis. Dr. Still’s previous paradigm of cause and effect was challenged. The change in approach to illness and healing that Still experienced due to this crisis led him to open a school in Kirksville, Missouri, and to begin to train physicians in the manual medicine technique of osteopathy. The basic tenets of osteopathy included the connection between structure and function and the idea that the body is a unit that has the ability to self-correct. Dr. Still also eschewed the use of pharmaceuticals in treatment based on his prior unsatisfactory observations.4
One of his students, Dr. William Sutherland, continued the development of osteopathic medicine, taking it in the cranial direction. Dr. Sutherland developed techniques to release restrictions at the cranial sutures and articulations, beginning the practice of cranial osteopathy. He observed a cranial rhythm generated from the “Primary Respiratory Mechanism.” Dr. Sutherland equated the mobility of the cranial bones with the health of the craniosacral system (Upledger, 1983).
In the 1960s, John Upledger travelled from Michigan to Kirksville to study osteopathic medicine. Once in practice, a challenging case resulted in interesting lessons. Upledger had the opportunity to assist a neurosurgeon by stabilizing the dura mater as the surgeon ran his scalpel along its surface. What he noticed was that the dura mater had an intrinsic, rhythmical movement not attributable to any of the other rhythms being measured in the operating room. Thus began a lifelong relationship with the craniosacral rhythm (CSR), a rhythm that Dr. Upledger hypothesized originated in the ventricles of the brain. The two phases of the CSR represent the cyclical production process of the cerebrospinal fluid (CSF). Recognition of the importance of the role played by the dura mater, both intracranially and extra-cranially, is one of the many contributions that Dr. Upledger has made to the evolution of Still’s work.
CRANIOSACRAL THERAPY TODAY
The present-day techniques of craniosacral therapy address connective tissue restrictions throughout the body, prioritizing “lesions” in order to facilitate release of the primary cause of dysfunction. The CSR is used as a feedback mechanism and measuring tool for the mobility of the laminar connective tissues of the body. As the dura mater forms, the walls of the venous sinus system and the intracranial membrane system, releasing restrictions of both the dura and its bony attachments, allow access to both the cerebral vasculature and the intracranial infrastructure.
CONCUSSION
According to the American Academy of Neurology, concussion is defined as “trauma-induced alteration in mental status that may or may not involve loss of consciousness.”5 It was thought that children were less affected by concussion than adults due to their increased capacity for neuroplastic change. However, children and teenagers are more likely to have more diffuse injury to the brain as well as prolonged brain swelling due to an increased sensitivity to changes in cerebral blood flow and metabolic dysregulation.6 This is particularly concerning, as one estimates that up to eight per cent of high school athletes suffer concussion (Kirkwood et al. 2006).
Understanding the scientific mechanisms behind concussion has been daunting, as diagnosis has been based on the subjective reporting of the injured individual. A multitude of quantitative tests have been developed, including neuropsychological testing with baselines pre-injury, performed again at the time of an athlete’s injury, and on-field memory tests such as the King-Devick test using numbers on cards. These tests have not clarified which structures of the brain are involved or the degree of severity of injury. Computerized tomography (CT) has been used in the past, but the imaging was generally “normal,” providing inconclusive quantitative evidence of injury.7
The magnetic resonance imaging (MRI) technique of diffusion tensor imaging (DTI) has helped with the identification of diffuse axonal injury (DAI), or injury to the subcortical white matter.8 These diffuse axonal lesions have been attributed to shear strain and tissue deformation caused by the rotational accelerations of the brain as an external force is applied to the head (Marata et al. 2011). The shear strains and tissue deformations of the primary biomechanical injury and resultant edema may be followed by axonal degeneration and neuronal cell death, secondary to the original injury. Due to the way in which the brain is connected via basal-frontal tethering, rotational acceleration of the brain can be caused by either angular or linear acceleration of the head from a direct blow or through the effect of a whiplash injury (Marata et al. 2011).
POST-CONCUSSION SYNDROME
PCS is defined by the World Health Organization as persistence of three or more of the following symptoms after head injury: headache, dizziness, fatigue, irritability, insomnia, concentration or memory difficulty.9 This diagnosis is usually reserved for patients whose symptoms persist for more than three weeks.10 It is possible that patients with PCS have semipermanent brain injury and that their diagnosis will change from concussion to minor traumatic brain injury (Willer et al. 2006). The symptoms have been further separated into three categories: somatic, emotional and cognitive (Karceski, 2011). Some researchers include a fourth category, sleep, to describe sleep-related issues. Some of the same symptoms seen in PCS have also been reported in patients with chronic pain.11 The effects on the autonomic nervous system (ANS) after concussion include altered heart rate variability (HRV), a measure of the variability of rhythmic oscillations in heart rate.12 HRV is a reflection of the parasympathetic-sympathetic nervous system balance.
| Case Study A 24-year-old male, who was an East Coast Hockey League centreman, was seen four months after suffering a concussion during a game. The impact of his opponent’s elbow contacting the right mandible resulted in loss of consciousness and brought an end to his hockey season. The patient presented with a myriad of familiar PCS symptoms, which were exacerbated by watching television and texting. On assessment, restrictions in range of motion were noted at the right parietal suture, and tightness was palpated in the falx cerebri. Treating this area not only resulted in quantitative changes in the patient’s perceived processing speed but also facilitated his ability to socialize. Treatments continued on a weekly basis and the intensity of symptom flare-ups decreased. Participation in low-intensity aerobic activity followed, with the goal of returning to symptom-free training. |
TREATMENT WITH CRANIOSACRAL THERAPY
Depending on the level of expertise of the practitioner, assessment of the patient would include evaluation of the craniosacral rhythm (CSR) for symmetry, quality and amplitude. This would be particularly relevant concerning the movement of the bones of the cranial vault. A more advanced therapist should use the “arcing technique” to locate the primary lesion site and to precisely locate tension patterns within the intracranial membrane system.
In an acute concussion injury, the focus should be on releasing any external forces that have affected the cranial bones and/or have been absorbed by the intracranial membrane system. These forces, depending on their strength, and the state of the tissue prior to injury, will tend to be absorbed by the body, leading to strain patterns within the collagenous portion of the connective tissues. These membranes are intimate with, and surround and separate, the brain sagitally and horizontally.
Hypermetabolism and hyperglycolysis in the initial phases of concussion, followed by insufficient metabolic activity, suggests the appropriateness of techniques for encouraging intracranial fluid exchange. Cranial pumping may be employed with the intention of facilitating the movement of cerebrospinal fluid (CSF) through the central nervous system. CSF bathes and feeds the brain and removes waste products, which helps promote homeostasis within the cerebral neurochemical environment.
Balancing the ANS is achieved through Dr. Sutherland’s very powerful technique of Stillpoint induction13. The compression of ventricle four technique (CV4) and Stillpoint technique stimulate a strong parasympathetic response giving the body a chance to move toward a homeostatic state. It is a technique to be avoided, however, if a concern exists regarding increased intracranial pressure.
CONCLUSION
Patients with concussion and PCS need to be treated to assist healing of the neurological, vascular and autonomic components of these injuries. Craniosacral therapy is one approach that may be applied by experienced therapists to facilitate this process.
References
- Belanger, HG, and Vanderploeg, RD. The neuropsychological impact of sports-related concussion: a meta-analysis. J Int Neuropsychol Soc, 2005;11:345-357.
- Binder, LM, Rohling, ML, Larrabee, GJ. A Review of mild head trauma. Part I: Meta-analytic review of neuropsychological studies. J Clin Exp Neuropsychol,1997; 421-431.
- Rimel, RW, and Giordani, B, et al. Disability caused by minor head injury. Neurosurgery, 1981; 9:221-228.1. Karceski, S. Concussion Neurology, 2011, Apr 26; 76(17): e83-5.
- Upledger, JE, and Vredevoogd, JD. CranioSacral Therapy. Berkeley: North Atlantic Books, 1983.
- Karceski, S. Concussion Neurology, 2011, Apr 26; 76(17): e83-5.
- Kirkwood, MJ, Yeates, KO, Wilson, PE. Pediatric sport-related concussion: a review of the clinical management of an oft-neglected population. Pediatrics, 2006;117:1359-1371.
- Arfanakis, K, and Haughton, VM, et al. Diffusion tensor MR imaging in diffuse axonal injury. Am. J. Neuroradiol. 2002;23:794-802.
- Marata, J, Lee and Stephanie W et al. A Unified Science of Concussion, Ann NY Sci, 2008, Oct;(1):58-66.
- Boake, C, and McCauley, SR, et al. Diagnostic criteria for postconcussional syndrome after mild to moderate traumatic brain injury. J Neuropsychiatry Clin Neurosci, 2005; 17:350-356.
- Willer, B, and Leddy, JJ. Current Treatment Options. Neurology, 2006;8:415-426.
- Smith-Seemiller, L, Fow, NR, Kant, R, Franzen, MD. Presence of post-concussion syndrome symptoms in patients with chronic pain vs. mild traumatic brain injury. Brain Inj. 2003, Mar;17(3):199-206.
- Leddy, JJ, and Kozlowski, K, et al. Regulatory and autoregulatory physiological dysfunction as a primary characteristic of post concussion syndrome: Implication for treatment. NeuroRehabilitation, 2007;22:199-205.
- Upledger, JE. Your Inner Physician and You. Berkley: North Atlantic Books, 1997.
Yonina (Nina) Chernick, BA Kinesiology ’87 from the University of Western Ontario and the University of British Columbia, trained at Sutherland-Chan School of Massage Therapy and opened private practices in both London and Guelph in 1991.Since then, she has studied craniosacral therapy and subsequently trained as an instructor and a Techniques Level examiner for the Upledger Institute. With Diplomate Certification achieved in 2000, she teaches courses, in both North America and abroad, to professionals from all areas of the health-care field.
This article was originally published in our Fall 2011 issue.
Print this page