
Features
Practice
Technique
5-step approach to treatment, management of degenerative disc disease
Through my 27 years of practicing massage therapy, I have had the opportunity to meet and treat many people with various conditions, including degenerative disc disease (DDD). This condition is often largely misunderstood or not understood at all.
March 14, 2022 By Mike Dixon
 Passive extension to the lumbar spine. Degenerative disc disease tends to be part of the natural aging process that we all go through
Passive extension to the lumbar spine. Degenerative disc disease tends to be part of the natural aging process that we all go throughWhen a patient receives a diagnosis of DDD, this does not mean that he or she is disabled, and that they are headed for a downward spiral of health and further spinal degeneration. In fact, DDD tends to be part of the natural aging process that we all go through, to one extent or another.
The aging body
As the human body ages, its mobility generally starts to decrease – the body feels somewhat stiff in the mornings and it’s generally harder to get out of bed. The first 30 minutes in the morning are the worst, and then the body starts to loosen or warm up. It also may be harder to find a comfortable position to lie in when going to bed. Turning over in bed might start to become a challenge. Even sex might be difficult at times.
These are all normal incremental symptoms people experience – usually starting at around 40 years of age.
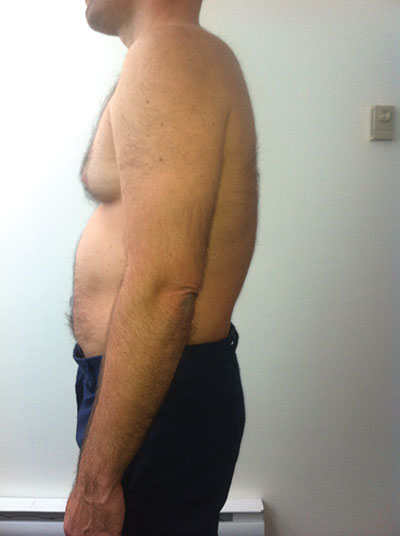 |
|
| Before passive extension treatment |
|
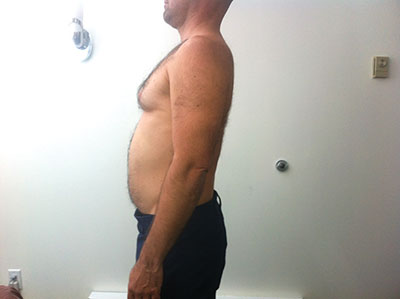 |
|
| After passive extension treatment Advertisement
|
When we are young, our intervertebral discs (IVD), which are situated between each vertebra in our spine, are full of a viscous fluid (jelly-like material). This fluid is called the nucleus pulposus. The nucleus pulposus is in the centre of each disc, whereas, the outside of the disc is a tough fibrous tissue called the annulus fibrosis. To give an analogy to this, discs are akin to a rubber tire on a car that is full of jelly, instead of air. The rubber tire is like the annulus fibrosis, and the air inside the tire is where the jelly like substance is.
As we age, the fluid in the disc becomes thicker and the annulus fibrosis degrades or weakens. The fluid becomes more like tar than jelly. Being a Canadian, I call this the “hockey puck syndrome,” as the disc become more like hockey pucks than tires full of jelly.
By the time we are 60, most of the fluid will have transformed into this much thicker tar-like fluid. The outside of the disc, the annulus fibrosis, may become bulging and misshaped rather than a nice round tire. The tires now may have bulges in them.
This scenario primarily happens in the low back, between the fourth and fifth vertebrae and the fifth vertebrae and the sacrum. These are the L4 and L5 discs or IVDs.
Discogenic pain (pain arising from discs) can be felt in the low back when these discs are affected.
The cervical spine, or neck, is often affected as well, usually between C4-C5, C5-C6 and C6-C7. So the discs of C4, C5 and C6 can generate discogenic pain in the neck.
This degrading process of the discs is known as degenerative disc disease or DDD.
In some people, as the discs degrade, the space for the nerves where they exit out of the spine – called the intervertebral foramina (IVF) – becomes narrow. This narrowing, called stenosis, can put pressure on the nerves that exit the spine where they travel to the arms or legs.
When stenosis occurs in the neck, it can cause pressure on the cervical nerves. This is often called a “pinched nerve” which causes pain radiating down the arm or leg. When pressure is applied to the nerves in the low back, or lumbar spine, it can cause a condition called sciatica, which is when pain radiates down the back side of the leg to the heel. When the pressure is applied to the nerve roots at the neck, or cervical spine, the pain travels down the arm and sometimes into the hand depending on which nerve is compressed.
The most common area of compression in the neck is the C5 nerve root, this causes pain radiating over the shoulder/deltoid and outside of the upper arm or lateral brachial region. The most common area of compression in the low back is the L5 nerve root, which causes the pain radiating down the leg to the heel.
These areas of pain or sometimes numbness are called the dermatomes, which are the areas of skin that are supplied by that particular nerve root. If the muscle is affected corresponding to the nerve root, this is called the myotome. Muscular weakness without any pain is possible when the myotome is affected and not the dermatome. If the dermatome is affected without the myotome, then pain or numbness is felt according to the nerve root being compressed. So the symptoms are dependent on what is being compressed and where.
These conditions are known as peripheral nerve stenosis, which means a decrease in the opening for the nerves exiting the spine (IVF). These conditions can be very painful and limiting to functional activities such as walking, running, hiking and daily grooming activities, like brushing the hair and getting dressed. These activities can pose a real problem for some people who have this affliction.
Treatment and management
I recommend a “five-system approach” to conservative treatment and management of DDD.
1. Education – The client/patient must understand the condition and the musculoskeletal effects of poor posture including sitting and standing postures. A healthy spine is a spine that has gentle curves from front to back (anterior to posterior). The low back or lumbar spine should have a small curve forward called a lordosis. The middle back or thoracic curve should gently curve backwards, called a kyphosis. The neck or cervical spine should have a gentle curve forward, called a cervical lordosis. When these curves are increased or decreased, the result is an enormous amount of stress on the discs (IVD) and the facet joints in the spine.
The three joints that support each vertebra allow us to move freely and in multiple directions. They are the two facet joints on either side of the vertebrae and the disc between each vertebrae. These three structures are known as the three joint complex. Each of these structures is designed to control and to attenuate specific loads onto the spine. When one of these structures is affected, the other two are also affected.
So when the disc is disrupted, so are the facets joints, and when the facets joints are disrupted so are the discs. This tri-complex is notably so connected that a mechanical disruption of any of the components of the three joint complex can lead to DDD and osteoarthritis of the spine.
Results that are seen on imaging (MRIs, X-rays, cat scans) are that DDD and osteoarthritis of the facet joints go hand-in-hand with each other. The term that is used is spondylosis.
2. Postural correction or mechanical extension of the spine – To reiterate, poor posture puts an enormous amount of pressure on the skeleton, especially the discs between the vertebrae. Gravity tends to pull us forward into a slumped posture. When you have a slumped or forward posture, there is a lot of pressure on the discs, which causes discs to slowly degrade. Simply put, the fluid within the disc creates bulges in the annulus fibrosis and causes disc degeneration. This degeneration causes spinal, back pain and sometime leg and arm pain.
The correction process is quite passive and done only to the patient’s comfort levels. The patient will lie face down on a specially designed treatment table, after receiving massage to the back muscles to soften the muscle tissue and reduce tension. The patient is covered with a blanket or towel. A broad strap is placed over the low back or mid back (the area to be treated). Slowly, the patient is extended (bent backwards) with the use of the moving parts of the table. This is done only to the patient’s comfort level. Traction is then applied to the spine to decompress the facet joints.
The position of extension allows the viscous fluid within the discs to shift towards the front side of the disc (anteriorly) shifting away from the back side of the disc. The shifting of the fluid takes the pressure off the backward side of disc (posterior wall) ligaments and supporting structures, allowing the body to regain the proper spinal curves and alignment.
3. Nerve mobilization and mechanical drainage of nerves – Pain that travels down a limb, whether it is an arm or a leg, usually means the nerve associated with that body part is likely being compressed at the nerve root level. The nerve root compression can lead to radiating pain, loss of motor control (muscular weakness) and or loss of autonomic function (blood vessel control) which affects the blood flow, which in turn can cause swelling in the limb. People that suffer from sciatica or a pinched nerve in the neck can well relate to these symptoms.
Nerve mobilization and mechanical drainage of the nerves help to decrease the swelling within the nerve to allow for better functioning of the neurovascular bundles. These techniques help to restore proper functioning to the nerves and therefore the quicker return to normal functional activities of daily living. These
techniques are not within the scope of this article but have been well described by the works of Dr. David Decamillis and
Dr. David S. Butler.
4. Exercise therapy for core stability and cardiovascular health – To support the postural corrections, proper strengthening and stretching exercises are indicated, as spinal alignment needs proper strength-length balance of supporting muscular tissue. Core stability exercises have been well documented to help the body recover from spinal conditions and musculoskeletal injuries. These type of exercises should be incorporated into an exercise program to maintain proper health and function of our bodies. Cardiovascular health benefits should not go without mention, as a strong cardiovascular system has a plethora of positive benefits for the human body including musculoskeletal and systemic health. The above three elements: stretching and strengthening, core stability exercises and cardiovascular training are needed for proper alignment, musculoskeletal health and overall healthy body conditioning.
5. Therapist-assisted maintenance for general spinal and musculoskeletal health – In today’s world, due to the ergonomics of the workplace, such as sitting and working on the computer and many other factors of activities of daily living, everyone needs some help, guidance and reminders for health. This should include mechanical correction of posture for the majority of the population. I call this the “spinal tune-up.”
Regular spinal maintenance is much better than treating acute injuries, such as a herniated disc or unrelenting back pain. Monthly or bimonthly corrective extension procedures to maintain spinal health and proper posture are recommended.
Mike Dixon, RMT, is a 28-year veteran of massage therapy. He is the author of the book, Joint Play the Right Way for the Peripheral Skeleton. He has been teaching since 1993 and has taught orthopaedics at the Boucher Institute of Naturopathic Medicine. He currently practices in Vancouver at the Electra Health Floor and in Tsawwassen, B.C., at Dixon’s Massage Therapy. He can be contacted through his company website www.electrahealthfloor.com.
This article originally appeared in our Winter 2015 issue. Posted 2015-01-07
Print this page