
Products
Workplace Allergens
I felt like I was sleeping in a bed of poison ivy. I woke up scratching, and psychologically, couldn’t stand being in my own skin anymore.
June 24, 2013 By Jules Torti
I felt like I was sleeping in a bed of poison ivy. I woke up scratching, and psychologically, couldn’t stand being in my own skin anymore. What innocuously began as a few itchy bumps on my wrist progressed to a systemic breakout of hives and welts. Blood tests revealed my allergen count to be triple the norm –and with my body cranking out cortisol double-time, I experienced random nose bleeds, hair loss, diarrhea, insomnia and a year-long lapse in my period. Hypo-pigmentation left me with white leopard-like spots on my back and legs.
 |
|
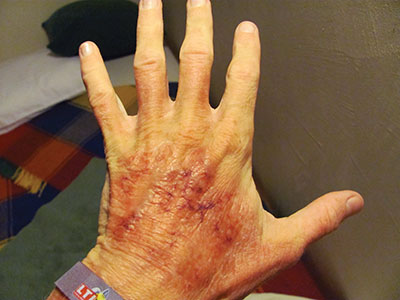
| Certain workplace related reactions can be controlled, or cured, with proper protective equipment. Gloves provided the answer to this skin irritation that was caused by bromine, a chlorine alternative often found in hot tubs and pools, including in facilities where RMTs may be working.
|
Pinpointing the root cause of my intense itching was nearly impossible. My doctor initially suggested it was a normal response to stress. I had just quit my job and moved back to Toronto from the west coast after a relationship had disintegrated. My dog had died. My bank account was thin after two extensive volunteer stints in Africa. I was sleeping on the floor of my brother’s apartment simultaneously trying to find a place to live and work. I was a country song waiting to happen.
Two months after finding employment at a Toronto spa, my hands were in an embarrassing condition. I would hide them in my pockets and hope that I wouldn’t have to shake anyone’s hand. They were raw, cracked and on fire—I looked like a crystal meth addict. I had tried an aggressive all-natural approach: soaking my hands in oatmeal for the colloidal benefits. I tried lavender, Argan and tea tree oil, baths in white vinegar and then lemon juice. Hot water made my skin crawl even more.
I had been a massage therapist since 1999, but refused to entertain the notion that maybe it was my career. I couldn’t justify that it was the grapeseed oil I was using. I switched oils and lotions, cleaning products, soaps, detergents and shampoos until I came to a dead end of hope.
Exasperated, I returned to my doctor. She gave me a prescription for a heavy dose of topical cortisone and a referral note for the dermatology specialist at Sunnybrook Hospital. There was a six-month waiting period just to see this doctor. In the meantime I visited Dr. Barbara Ho Ping Kong, a dermatologist who could see me sooner. She prescribed more cortisone and insisted I quit my job. “I see many massage therapists like you. You will continue to be like this unless you wear gloves or teach or quit massage.”
A full year of suffering later, and unable to digest Dr. Ho Ping Kong’s dose of reality and advice, I went to Sunnybrook for further testing. I had 60 different allergens placed in Smartie-sized discs taped to my back for a three day period. Samples of oils and lotions I had been using to massage with were also applied. After three uncomfortable days of not showering and living with potential allergens glued to my back, I returned for the conclusive appointment.
Apparently I was allergic to ylang ylang. Which I never used and which wasn’t in any product that I used at home. I was totally defeated.
Eventually I discovered it was the bromine (a chlorine alternative, often used in indoor pool facilities) used in the salt water pool and hot tub at my workplace. I routinely massaged wet clients who had just stepped out of the waters. Finally, the constant irritation and flare-ups made sense. Once I started wearing gloves, the itching was resolved.
I have no choice but to wear nitrile surgical gloves during treatments now – even though I have removed myself from the environment with the bromine exposure. Three years of subjecting myself to the allergen and chronic use of cortisone resulted in a severe hypersensitivity.
BUT I KNEW I WASN’T ALONE . . .
Norine Blyth of Uxbridge Massage Therapy Studio has been practising for 25 years. Twelve years ago, after a stressful marital separation, she developed a form of eczema isolated on one hand. Massage cream seemed to irritate it and her emotional guilt to potentially spreading it to her clients compounded the issue.
“At first when everything started I was devastated, I couldn’t get my head around the whole thing about not being able to work, especially since I had just become single and needed to work more than ever. I would take time off when my hand flared, then tried one glove but clients didn’t like it and I didn’t like it either. We both could feel the difference between the two hands. I considered quitting the profession altogether. A girlfriend of mine said, ‘Just wear them on both hands’ – so the rest is history. I wear gloves 99 per cent of the time. I don’t get many flare-ups anymore, but feel it is safer for both parties as the skin is the largest organ.”
Blyth was originally embarrassed to tell clients that she had to wear gloves. “I would make a joke about it by saying, ‘I won’t play doctor.’ Some clients would look at me weird, but at the end of the massage they would say they didn’t even notice them.”
With permission, I e-mailed one of Blyth’s clients, PJ Moore, for her thoughts. “My initial reaction to my first massage with gloves was hesitation. I thought it might feel cold or that the gloves would stick to my skin and not feel as soothing. It did make me think of condoms or the excessive use of bacterial cleaner versus the way I grew up with the five-second rule. Applied with the right amount of oil or lotion though, the gloves glide over your body like a slip-and-slide ride. No worries! As I relaxed and enjoyed the massage, I thought about how much safer it must be for Norine.”
Ashley Winnington-Ball, a customer service agent at Body Blitz Spa, didn’t notice any initial difference upon receiving a gloved treatment. “I occasionally heard an unrecognizable sound which I realized at the end was from the gloves. That was a bit distracting. Also, not having been told at the beginning why the therapist was wearing gloves made the revelation a little awkward. I was thinking, “That’s weird. Why is she wearing gloves? Is it something about me?”
ADDRESSING THE ISSUE
What is the best protocol for broaching glove-wearing with a client before a treatment? This is a discussion that each therapist will have to decide individually or in conjunction with their employer. And, will they still consent to the treatment or opt to cancel? With a long-standing client base, the majority of Blyth’s clientele were accepting of the gloves. She’s never had anybody flat out refuse treatment because of it – or, as she chides, maybe they just never came back.
For MT Trish Burkholder, periodic reactions to additive and preservative-laden soaps and lotions at clinics where she was employed were the first red flag. “I have also been lucky enough to get both an abscess and a staph infection from clients and both found their way into me via a small ‘scratch’ in my hand. I also know that some clients react negatively to the lotions as well.” Recovering from her staph infection knocked her out of work for a month. She continues to wear gloves, but not every day.
Alisha Brady, who graduated a year and a half ago, had a severe flare-up that resulted in her having to take six months off work with no real avenue for alternative income. Despite trying to find an alternative to cortisone (diet change, naturopath), she resorted to using it and wearing gloves as a precaution in the end. Stress and the constant friction of massage continually exacerbate her eczema. “I did and still do consider a career change. If the general population were more accepting of gloved therapists, I would not be seriously considering a transition – but at this point, I wonder how I can have a career as a gloved therapist.”
Brady has found compassion from clients who also suffer from eczema: they understand her need to protect herself from further irritation. Many don’t even realize she is wearing gloves until they turn supine.
PROTECTING OURSELVES AND OUR CLIENTS
Both Blyth and Brady were surprised that our safety as massage therapists is so easily compromised. Wearing gloves is a welcome barrier when clients present with undiagnosed rashes, warts, boils and blemishes. Gloves are a more sterile approach for both parties. Blyth wonders why gloves haven’t been mandated by her College for client safety. On the same topic, Brady remarked, “I find it quite odd that massage therapy would be the one health-care profession where the therapist would be assumed not to wear gloves during treatment considering the extent in which we work intimately with the client.”
A DENTIST WEIGHS IN
For Toronto dentist Naila Ladha, wearing gloves “is essential. There’s no compromise.” The transfer of disease is high with exposure to saliva, blood and vasculature. She understood the necessity of wearing gloves for obvious indications like warts, severe eczema or psoriasis. But, if the epidermis is our body’s natural barrier against disease and infection, why would gloves be necessary otherwise? Ladha was more concerned about the sensation that would be transferred by a massage therapist wearing gloves than she was about protection. “Wouldn’t nitrile or latex gloves pull on the skin of clients if not properly oiled up? Would the client be able to feel the warmth of your hands through the gloves?”
UNEXPECTED FINANCIAL SETBACKS AND JUMPING CAREERS
Melanie Horvat had worked as an esthetician at the Langdon Hall Country Hotel and Spa for a decade when the spa introduced a new product line for facial, body and nail care. Horvat routinely performed aromatherapy massages during Vichy body scrub treatments. Itchy blisters on her palms, and even itchier, swollen eyes led to her taking time off work. She returned a week later to find the reaction only intensified and spread to her feet, legs and buttocks, and crawled up her forearms.
Horvat’s hands, often immersed in water, became cracked and were prone to bleeding. She started wearing vinyl gloves to protect herself. She wore long sleeves to hide the unsightly weeping wounds on her forearms. After taking an additional week off one month later, the rash seemed to completely resolve with frequent oatmeal baths and Aveeno. When she returned to work the rash appeared again, with a vengeance. A doctor’s recommendation led to modified duties at the spa and decreasing her exposure to product. Working strictly at the reception desk for a week, her rash spread systemically and, as Horvat explained, “I looked like I had second-degree burns.”
Her doctor prescribed prednisone, while a patch test at St. Michael’s Hospital in Toronto indicated an allergic reaction to fragrance and perfume, matching four ingredients in the product line she had been using.
During the time between allergy tests, Horvat was offered a position at the front desk of the hotel so she could avoid airborne exposure from the confines of the spa. However, clients wearing cologne and scented cleaning products put her over the edge, again. Luckily for Horvat, an occupational health specialist with WSIB sent her for an occupational assessment after deeming her workplace unsafe. She qualified for retraining as a cardiovascular technician.
Unfortunately, many registered massage therapists are self-employed and unable to qualify for such funding or support for educational pursuits. Those unable to work due to overexposure in the massage industry should plan seriously for the possibility that they may face serious financial repercussions or be forced to pursue a new career.
HOW WILL THE COLLEGE RESPOND?
Currently, the College of Massage Therapists of Ontario’s policy on this issue can be found on the College website, and is as follows:
“The College’s Communication/Public Health Standard # 15 – Use of Personal Protective Equipment During a Treatment states that it is the responsibility of each registrant to determine the conditions where it would be necessary to utilize protective equipment. Conditions include:
- a client or a therapist with a recognizable contagious condition that might be spread by contact or inhalation during the massage therapy treatment
- a client who requires intra-oral treatment as part of their treatment
- a client or therapist with non-intact skin, or open or healing lesions that would be vulnerable in the course of providing massage therapy treatment.”
Although this policy is a basic premise, given the myriad situations in which RMTs and clients may be at risk, I believe there’s a necessity to create stronger legislation for RMTs on the topic of wearing protective gloves. The issue needs to be addressed openly and policy needs to reflect, clearly, the urgency of the matter.
With increasing numbers of massage therapists being afflicted by workplace allergens and debilitating skin issues due to overexposure, will our Colleges take a stand? Where is the appeal in entering a profession where your own personal wellness is sacrificed? What options are there for massage therapists forced into a sudden career change? Will employers welcome new MTs who find it necessary to wear gloves during treatments? Will the public learn to accept that gloved treatments are the safer option?
I imagine there will be a rejection period, just like the resistance to any movement requiring radical change: mandatory bike helmets, mouth guards in sport, peanut-free lunches in elementary schools.
While other health-care professionals, hairdressers, fast-food chain employees and tattoo artists wear gloves for occupational health, it’s unsettling that our “hands-on” profession is still leaving everyone rather exposed.
Jules Torti has been an RMT since 1999 and an industrious freelance writer since age six. She has worked in hotels and spas in both Ontario and British Columbia. In between massage engagements, she travels to Africa to be with chimpanzees and writes about her zany travels for Matador Network.
Print this page