
Features
Management
Operations
Essentials of Assessment: Winter 2003
The assessment of the joints of the cervical spine requires a minimum of three different testing procedures, after having done Range of Motion testing. Each of the three tests matches the three versions of synovial joints found in the cervical spine.
September 23, 2009 By David A. Zulak MA RMT
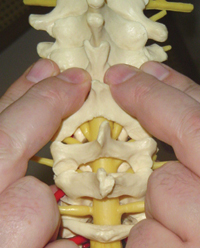
The assessment of the joints of the cervical spine requires a minimum of three different testing procedures, after having done Range of Motion testing. Each of the three tests matches the three versions of synovial joints found in the cervical spine. Anatomically, the cervical spine is divided into the “upper quadrant” the “lower quadrant.” The upper quadrant is composed of the occiput-C1-C2 – with the 1st and 2nd cervical vertebrae being “atypical.”
|
|
|
Essentials of Assessment
The upper quadrant is composed of the occiput-C1-C2 – with the 1st and 2nd cervical vertebrae being “atypical.” The lower quadrant is made up of C2-3-4-5-6-7. C2 & C3 make up a transitional point between the upper atypical and the lower ‘typical’ vertebrae, and C7 and T1 making up the transition point between the cervical and the thoracic vertebrae.
For a quick test for the Occipital-Atlas (“OA”/O-C1), the therapist should be at the head of the table while the client lies supine. Ask the client to do the following actions, but they should try to “Keep the back
of your head on the table; try not to lift your head while doing this, just let your head slide along the table.”
Have the client tuck the chin in as much as possible. The therapist is looking for the chin to deviate to one side or the other. Then have the client tip their head back as far as they can. The results of deviations of the chin are the result of one of the two OA joint surfaces being ‘fixed or stuck.’ As fixed the joint then becomes a pivot point around which the head moves:
In flexion: the opposite side as the deviation is fixed (e.g., Right side is ‘stuck closed’ in extension)
In extension: the same side is fixed (e.g., Right is ‘stuck open’ in flexion)
 |
 |
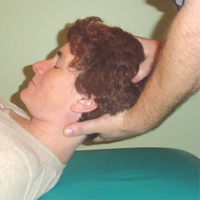
For the testing of the upper quadrant’s Atlantoaxial joint (“AA”/C1-C2), the therapist can stand at the head of the table while the client is laying supine on the table. Gently, but firmly, take hold of the client’s head with two hands and lift it into full flexion. The chin should be tucked in so that the upper as well as the lower quadrants are in flexion.
Now, support the cervical spine with one hand. This hand should have C1 or C2 in the web space between the thumb and index fingers, and initially you can have the occiput resting in the palm of that hand.
Taking the free hand, now place it on the ‘crown of the head’ (occiput-parietals area). All this time the client’s cervical spine is held in flexion. Now that the head is supported with one hand at the ‘crown,’ tilt the hand holding the spine so that the palm is no longer touching the occiput, but the spine remains supported by the web of the hand.
So, just to make sure you are in the right position: you are standing behind the client’s head with your elbows out. The hand under the client’s neck is thumb up (or facing away from you), and the hand on the clients head is thumb down. Holding the client’s head in flexion as far as is comfortable for them stretches the facet joint capsules and limits their ability to flex or move in any direction any further. The lower quadrant is now “fixed in place”
As 50 per cent of the cervical spines rotation comes from the Atlas rotating around the dens of C2 (the Axis) we can use the upper hand on the head to rotate the head left and right. We should get approximately 45 degrees in either direction.
If we get less on one side than the other, then we know that the AA joint is involved in the client’s loss of rotation.
- If this loss equals the total loss seen in Active Free ROM testing then the AA joint is the area to work.
- If it is only part of the loss seen in AF testing then both the upper and lower are contributingto the loss of rotation.
- If the AA appears normal, but AF or Passive Relaxed had showed loss of rotation, then that loss should be coming from the lower quadrant (the client’s facet joints and/or operative musculature).
- Note: if rotation to one side seems excessive, and rotation in the other direction appears limited, this may mean that the C1 vertebra (the Atlas) is ‘rotated’ on C2 (the Axis).
These two tests give us a good testing protocol of the cervical spine’s upper quadrants.
Now, to test the lower quadrant we are going to employ the motion of “translation.” As the facets are plane-gliding joints, (roughly on a 45 degree angle with the anterior portions pointing upward), they have the ability to slide side to side or “translate.”
Just as they have the ability to glide anterior-superiorly (flexion, opening the joints) and glide posterior-inferiorly (extension – and hence ‘closing the joint’ or approximating the joint surfaces).
In translation of the cervical vertebrae through the paired facet joints we are testing “side-bending.”
As side-bending and rotation are always coupled in the cervical spine, we are also therefore testing rotation.
Now, if we find restrictions while the cervical spine is in flexion and is translated that will imply that the restriction is due to a facet that will not open.
If we hold the spine in extension and perform translation and we find restrictions, then that restriction is
due to a facet that will not close.
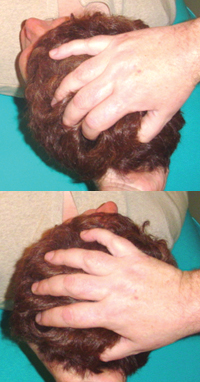
To do the test for each level of the lower quadrant from T1-C7 to C3-C2, begin by placing the index and middle fingers in the lamina groove on either side of the cervical spine, while the therapist holds/supports the head in the palms of their hands. The fingers need to be in the lamina grove (which is composed of the ‘articular pillars’ of the facets) and not on the tender TVPs.
Starting at the T1-C7 level have the fingers at the level of C7 ‘s transverse processes (TVPs) but in the lamina grove on either side. With the heels of the hands supporting the occiput translate or slide the head and the whole cervical spine as if one fixed structure from side to side.
Holding all of the cervical segments fixed and moving over T1 places the movement specifically between C7 and T1’s facet joints.
Now the therapist moves up one level, with the finger tips in the lamina groove adjacent the TVPs of C6. Translate through the facet joints of C6 & C7. Work your way all the way up. At the lowest level there should be a side to side movement of an inch or so, equal to each side. As the therapist moves up the movement to either side will become greater, but should remain equal to each side.
- When the head is held flexed and translated the restriction is to the opposite side to which the spine is being translated. If translating to the left and the movement is restricted, then the restricted facet is on the right.
- When the neck head is extended and translated the restriction is on the same side as the direction showing resistance to movement.
- If this example is done as translation while the neck is flexed then the dysfunction is on the left side – C3-C4 facet on the left is fixed closed (or ‘extended’). In flexion = dysfunction is opposite to side being translated to.
- If in this example the translation is done while the neck is extended then the dysfunction is on the right side – C3-C4 facet on the right is fixed open (or ‘flexed’). In extension = dysfunction is on the same side as being translated to.
This translation can occur through C1 (by holding only the occiput). This tests the approximately 3 degrees of side-bending available. The OA joint can be tested in flexion and extension to locate the area of dysfunction. The above rules apply.
• Next Article: Some variations and treatment techniques that mirror the assessment techniques.
* The client can be seated, but it is harder to have true passive movement as the client can not truly let go of the cervical and related musculature.
• Fred Mitchell Jr. D.O. holds that the translation palpation of the OA joint gives more pertinent information then the general test for the OA joint presented at the beginning of this article. See The Muscle Energy Manual, Vol. 1, 1995.
Print this page