
Features
Practice
Technique
Essentials of Assessment: Fall 2004
the shoulder joint complex – made up of the glenohumeral (GH), the acromioclavicular (AC), the sternoclavicular (SC) joints and the scapulothoracic articulation (STA) – requires a highly organized testing protocol or procedure. The shoulder is definitely prone to multiple lesion sites, even with the most “simple” injury.
September 25, 2009 By David A. Zulak MA RMT
testing of the scapulothoracic & scapulohumeral motions
the shoulder joint complex – made up of the glenohumeral (GH), the acromioclavicular (AC), the sternoclavicular (SC) joints and the scapulothoracic articulation (STA)1 – requires a highly organized testing protocol or procedure. The shoulder is definitely prone to multiple lesion sites, even with the most “simple” injury. To bring a shoulder back to health; or to prevent or limit the chronicity of a “bad shoulder,” as many sites as possible of dysfunction and sources of pain (local or referred) need to be found and treated.
The focus of this article concerns what is referred to as scapulothoracic motion and especially the coupled motions of the scapula and the humerus, (scapulohumeral motions).
Having the results of active free range of motion testing with respect to impairments found in various ranges of motion testing of the shoulder, the therapist will also want to assess the various joints in combination: how they work together.
The focus of this article concerns what is referred to as scapulothoracic motion and especially the coupled motions of the scapula and the humerus, (scapulohumeral motions).
It should be mentioned that, during active free range of motion testing of the shoulder, the therapist can be checking the function of the SC and AC joints as well. This is achieved by palpating the motion occurring with the clavicle during certain portions of active ROM testing of the shoulder.
This will help to assess more thoroughly where possible sources for shoulder restrictions are coming from; especially those that appear as the arm rises above shoulder height.
This palpation of the clavicle during shoulder motions gives us clues as to how much the SC and AC joints may be involved in shoulder dysfunctions or pain.2
Note: Later, under passive range of motion testing, the SC & AC joints will be specifically assessed, and still further investigated by various stress tests while doing specific (“special”) orthopedic testing.
Such motion palpation, as suggested above, and with what follows, basically only requires the client to repeat each shoulder range of motion two or three times while the therapist observes and palpates various portions of the shoulder complex during those movements.
My preference is to palpate clavicular motion (hence SC and AC joint functions) when doing general shoulder movements.
Leave the ROM testing of the scapula and scapulothoracic motions for the last stage of the active free testing because it uses some repeated active free motions. It also includes a ‘guided’ or assisted movement, and passive movement. Doing these at the end of active free ROM testing provides a bridge to the passive motions done next in the protocol.
First, the Four Active Free Ranges of Motion of the Scapula:
1. Elevation: Instruct the client to start with their arms at their side. Have the client shrug their shoulders. The scapulae should rise up on the thoracic cage. The inferior angle of the scapula should not swing out laterally. This would imply that the superior aspect of the scapula is adhering to tissues surrounding it. The therapist needs to see/palpate the superior angle of the scapula move up. Also, try to prevent the client from rolling their shoulders forward as this ‘trick’ can give the appearance of elevation, when it is actually protraction.
2. Depression: Have the client bring their shoulders down, not back, as if assuming a military stance. If you like, have them reach straight down toward the ground. Again, the inferior angle of the scapula should move only slightly lower.
3. Protraction: Have the client roll their shoulders forward. The scapula should slide laterally, increasing the space between the spinous processes of the vertebral column and the medial border of the scapula. It is usual for some rotation of the scapula to occur, as the inferior angle tends to move further laterally than the more tethered superior angle.
Protraction occurs primarily when one reaches forward. Ask the client to do just that – “reach forward with both of your arms, as if your hands are trying to grab something just beyond your reach.”
If done with both arms at once, the client is less likely to “cheat” by twisting their upper body.
Note: the therapist will often observe that the ‘resting’ scapula is, to some degree, already starting in
a protracted state – by how much can be gauged by how much further away from the spine the lower angle of the scapulae is as compared to the superior angle. ‘Natural posture’ with the arms at the side, always finds the lower angle somewhat farther from the spine, but experience will tell the therapist when this is too much.
This may already be noted previously by (postural) observation.
This may also be noted when the client displays good internal rotation coupled with restricted external
rotation, i.e., the client is not starting from an anatomical neutral position, but from a protracted position.
4. Retraction: Ask the client to try to bring their shoulder blades together, thereby decreasing the distance between the medial or vertebral border of the scapula and the spinous processes.
Note: if when the medial border of the scapula moves closer to the spine that, as it does so, it appears to be parallel to the spine. If the inferior angle remains further away, suspect a weak (stretch/ lengthened weakness) of the lower traps. It is common for this weakness to also be the result of inhibition due to an upper cross syndrome (Vladimir Janda).3
Now, to the principle topic of this article: the coupled movements of the scapulae & the glenohumeral joints
If restrictions are detected in general range of motion testing of the shoulder girdle or of the scapulae (as described above), then the following testing protocol for scapulohumeral motions is very informative. This testing will provide information that can make the cause of shoulder injuries, especially chronic dysfunctions, clearer and justify the impairments that the client’s shoulder is displaying.
The range of the scapula on the thoracic cage during shoulder movements (hence the name scapulothoracic motions or articulation) is usually measured by its relation to glenohumeral abduction.
This is represented by a 2:1 ratio. Every 3º of abduction of the arm is comprised of 2º of movement in the glenohumeral joint and 1º of movement in the scapulothoracic motion.
Remember, this is a generalized statement considering the total movement of both the scapula (60º) and the glenohumeral joint (120º) provide the 180º of shoulder abduction.
I have designed three tests that help to sort out dysfunctions that are made clear when observing this specific coupling of the humerus and the scapula. The first of these is a cross between active free and active assisted.4 Have the client move against gravity, you control the speed of the movement. If the client goes through the movement of abduction very slowly, this test can reveal the process or timing of engagement of various muscles in and around the shoulder girdle.5
PROCEDURE: TEST ONE
While standing behind the client’s shoulder that you are about to test, grasp the inferior angle of the scapula between your thumb and your index finger of your hand that is closest to their spine. With your other hand, grasp the client’s upper arm and have the client slowly begin to abduct it.
Normally, scapular movement does not occur within the 15º of abduction. Be sure to distinguish the twitching of scapulohumeral muscles “turning on” (becoming ready to do their job as scapulae stabilizers).
To initiate abduction, the client has engaged or “turned on” the supraspinatus and the middle fibres of the deltoid. Other muscles have engaged to stabilize the scapulae, and so, no motion occurs yet.
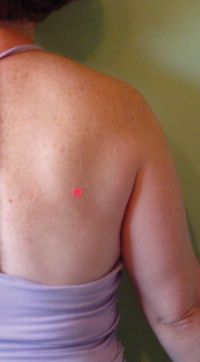
After 15º to 30º of abduction you will notice that the inferior angle of the scapula (that you are holding onto, while allowing movement) will swing laterally, following the movement of the arm. Between 15º to 30º of abduction, the muscles that are meant to stabilize the glenohumeral joint6 during movement, or weight bearing, are taut enough (engaged and slightly stretched) to begin to pull along the scapula to which they are attached, which will follow the arm (humerus) into abduction (or other movements of the glenohumeral joint).7 The scapula must move so that the rotator cuff muscles can remain efficient in stabilizing the GH joint. From 15º or 30º to approximately 90º, there is roughly the 2:1 ratio of movement between the glenohumeral joint and the scapulothoracic articulation.
As the arm approaches 140º of abduction, the motion of the scapula begins to equal and then exceed the movement from the GH joint.
For the arm to continue to abduct (normally) past 90º the humerus rotates 90º on its axis moving the greater tubercle out from under the acromial arch.8 If the humerus does not rotate, then the range can be restricted to 120º. During this rotation of the humerus the clavicle must also rotate posteriorly at least 50º along its axis. If the clavicle does not rotate then the movement will also be restricted to 120º.9
A) If you notice the scapula begins to move or engage almost immediately upon abduction (before 15˚), then you may suspect:
1) “Frozen Shoulder” or adhesive capsulitis10
2) tight or spasming or contractured muscles of the rotator cuff11 or
3) very weak or inhibited rhomboids and middle & lower trapezius.
Frozen Shoulder is ruled out by having noted during active free ROM if the client has a capsular pattern of restriction of the glenohumeral joint: external rotation was highly restricted and abduction quite limited, (there may also be slight loss of internal rotation and flexion during the most acute phase of frozen shoulder).
The latter two conditions (2 & 3), causing premature movement of the scapula, can be noted with observation and palpation. They could be further investigated with specific muscle strength testing.12
Conversely, if there is no movement of the scapula until after 30˚ of abduction, (45 to 50˚, for example) then investigate if the muscles that stabilize the glenohumeral joint, ‘rotator cuff muscles,’ are somehow inhibited or injured. Again, we would use strength testing (as mentioned above). It is possible, but rare, for the rhomboids to be so tight or in spasm as to prohibit movement. Palpation would be informative.
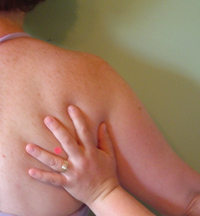
PROCEDURE: TEST TWO
The second test administered for scapulothoracic motion is a Passive Relaxed Movement.
As a passive movement, the client’s musculature is not engaged and so we are testing the inert or non-contractile tissues of the shoulder. In this case, primarily the joint capsule. This test will help substantiate an assessment of adhesive capsulitis.
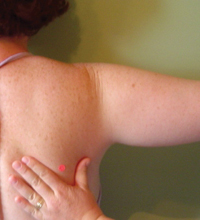
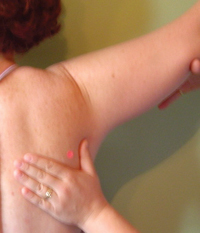
While standing behind the client’s shoulder, lightly grasp the inferior angle of the scapula between the thumb and the index finger, (with the hand that is closest to the client’s spine). With your other hand grasp the client’s upper arm and ask the client to relax as much as possible and move their arm slowly into abduction. Remember to externally rotate the humerus so that the greater tubercle does not impinge under the acromion and prevent full abduction.
Normally, the arm should be passively abducted to 70-90˚ before the scapula begins to move. This happens because the supraspinatus and middle fibres of the deltoid have not been engaged (or “turned on”) by the client who is letting you lift their arm.
Therefore, the ‘rotator cuff’ should not engage either. It is now the fully stretched joint capsule of the glenohumeral joint, along with the stretched but relaxed scapulohumeral muscles, that causes the scapula to be dragged along after the arm.
If the scapula is clearly moving before 70˚ of passive abduction is reached, then there may be:
A) a capsular restriction, or contracturing musculature;
B) spasming of the ‘rotator cuff’ muscles, individually or jointly, as these tissues are stretched;
C) hypertonic scapular muscles, including muscles with Trigger Points (TrPs) can twitch and engage too soon, and thereby cause scapular movement to occur; (i.e., these muscles will not allow true passive movement to happen). Palpation here can help. Look for the classic local twitch response of a TrP.
PROCEDURE: TEST THREE
The third test, is specifically for glenohumeral movement alone.13
Without scapulothoracic motion, 120˚ of abduction is the maximum expected movement of the glenohumeral joint. If this 120˚ can be reached, we can be confident that any loss of range of motion is not coming from the glenohumeral joint.
The scapula and its musculature becomes the prime suspect, (as long as we have ruled out the SC and AC joints prior to this point in our testing). This test should be done actively as well as passively.
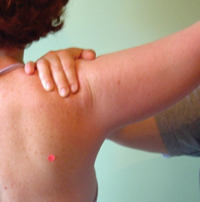
While standing behind the client’s shoulder lay your hand, that is closest to the client’s spine, on the client’s acromion. With the other hand, grasp the client’s upper arm and ask the client to relax allowing their arm to be passively abducted. It is wise to begin with the arm already externally rotated. Prevent the scapula from moving by adding a firm downward pressure over the acromion.
A) Before lifting the arm, have the client extend their arm with the palm facing away from their body and ensure the palm remains facing up as the arm is passively abducted, or
B) If the arm is heavy, have the client’s elbow flexed with the palm of their hand facing forward.
 As mentioned previously, this testing should be repeated with the client actively moving the arm into abduction. This will help clarify the results found.
As mentioned previously, this testing should be repeated with the client actively moving the arm into abduction. This will help clarify the results found.
If the client reaches a full 120˚ we can be confident that any loss of range of motion that was noted during general active free ROM testing of the shoulder is probably not coming from the glenohumeral joint. Rather, the restriction of movement is coming from the tissues in which the scapula is contained. The scapula may be adhering to the surrounding muscles and tissues in which it normally moves if there is scar tissue or fibrosis causing adherences in these tissues.
Scapulothoracic movement could also be restricted by spasming of, or with the presence of trigger points in the rhomboids and middle trapezius. Again, palpation and muscle testing will be of help in sorting this out.
Of course, if the client’s arm can not reach 120˚ then we need to estimate if the shortfall equals the loss seen in active free motion.
- If the loss of motion of the GH joint specifically equals the loss seen previously in general active free range of motion testing of the shoulder, then the GH joint is our culprit (again, as long as we are fairly confident that the clavicle is moving well and thus the SC and AC joints can be ruled out from the list of suspects). Certainly, the scapula is fairly free of suspicion.
- If loss of motion here is seen only actively and not during the passive version of this test, then the musculature is involved in the restriction.
- If the restriction is fairly equal in passive or active testing then we need to do a thorough passive testing of the GH joint (including joint play assessment).
CONCLUSION:
Including these tests in your shoulder protocol are of great help in revealing a more complete picture of the impairments of the shoulder complex. All too often “rotator cuff tears” of the supraspinatus or infraspinatus are treated too specifically or narrowly.
Usually, a number of tissues and muscles are involved in any shoulder injury, and they all need to be tested. This will lead to more comprehensive treatments and a greater chance of preventing ongoing “mysterious” problems in the shoulder girdle.
REFERENCES
- See Hoppenfeld, page 23-25; Magee, pages 100-101.
- These tests of the SC and AC motion are concerned with rotation of the clavicle, which will be involved in the last 90˚ of motion during abduction. The clavicle itself should roll approximately 50˚ during full abduction or forward (hyper) flexion.
- See Massage Therapy CANADA, Winter 2003 Issue.
- Active assisted movements are intended to negate the affect of gravity on a limb or joint so that very weak or compromised muscles along with other structures can still be tested when the client is no longer strong enough to overcome gravity, or to do so would cause pain. Here we are not negating gravity, but rather controlling the speed of the client’s movement.
- This biomechanical investigation looks at what is often called the “kinetic chain.” This is the sequence of different muscles engaging one after another in a certain order whenever movement in a joint occurs; engagement that leads to a natural progression to other movements in other joints, or to stabilization of that joint or surrounding tissues or joints during a movement, etc.
- Here, the infraspinatus, teres minor, and subscapularis. Along with the supraspinatus they are referred to as “the muscles of the rotator cuff,” and their job as such is to stabilize and hold the head of the humerus into the glenoid fossa, (hence the glenohumeral joint). Because of this stabilizing work they are sometimes referred to as “active ligaments.”
- Other movements include reaching forward which includes protraction of the scapula, etc.
- See painful arc above.
- There are many people who can abduct almost to 180˚ without rotation of the humerus, and this represents a laxity and mobility in and around the acromial arch and glenohumeral joint connective tissue structures that does not need to be considered abnormal.
- When the scapula begins moving almost immediately, and you notice that abduction of the arm is not taking place at the glenohumeral joint but only by the sliding of the scapula along the thoracic wall, (to a total of 60˚ maximum) the client is said to be suffering from “Frozen Shoulder.”
- See note 14 above.
- See Kendal & Kendal, pages 107-111
- See Magge, pages 101-3.
Print this page